1. Introduction
The definition of wound infection is revised by the centers for Disease Control (CDC) in 1992, by creating the definition of “surgical site infection” [SSI] which prevents the confusion between surgical incision infection and traumatic wound infection. SSIs contribute to the morbidity and mortality which are associated with surgeries, although most of SSIs are superficial [1].
Surgical site infection (SSI) previously termed postoperative wound infection is defined as that infection presenting up to 30 days after a surgical procedure if no prosthetic is placed and up to 1 year if a prosthetic is implanted in the patient. Based on a survey data there were over 290,000 infections in hospitalized patients in the US in the year 2002 of these, SSI was estimated to be directly responsible for 8205 deaths in surgical patients that year. SSI results in patient discomfort, prolonged length of hospital stay and increased cost [2].
The risk of developing SSI is affected by many factors which includes the degree of microbial contamination of the operation site indicated by wound class as clean, clean contaminated, contaminated and dirty, and also by patient age, length of surgery, pre-operative shaving of the operative site, hypothermia and co morbidities e.g. diabetes and obesity [3].
Surgical site infections are about 20% of healthcare associated infections. Failure of wound healing result in developing SSIs which increases treatment cost as it increases hospital stay time, admission to intensive care unit and higher post operative mortality. For each infected patient hospital cost is estimated at US$3937, therefore surgeons and other healthcare professionals are interested in prevention of SSIs [4].
Surgical wound classification is an indicator for infectious risk assessment, perioperative protocol development and making of surgical decision. Wounds are classified into 4 classes clean, cleancontaminated, contaminated, and dirty wounds with postoperative rates of SSI as 1-5%,3-11%, 10-17%, and over 27%, respectively [5].
According to the Center for disease control (CDC) there are four types of wound class illustrated as following [6]:
| Clean | No acute inflammation or entry into GI, respiratory, GU, or biliary tracts; no break in aseptic technique occurs; wounds primarily closed |
| Clean contaminated | Elective, controlled opening of GI, respiratory, biliary, or GU tracts without significant spillage; clean wounds with major break in sterile technique |
| Contaminated | Penetrating trauma (<4-hr old); major technique break or major spillage from GI tract; acute, nonpurulent inflammation |
| Dirty | Penetrating trauma (>4-hr old); purulence or abscess (active infectious process); preoperative perforation of viscera |
The aim of this prospective observational study is to assess the procedures of antibiotics use as prophylaxis of surgical site infections in pediatric patients in the pediatric surgery department, in a teaching university hospital, and the adherence of the hospital to the published international literature reviews about antimicrobial prophylaxis protocols.
2. Patients and Settings
2.1 Design
Observational Prospective study
2.2 Setting
Teaching University hospital, pediatric surgery department, the department consists of three units the ward, the ICU, and the operation unit. There is no pharmacy inside the unit. Drugs are dispensed weekly from the floor pharmacy to the nurse and stored in the stock cabinet.
2.3 Patients
Hundred surgical pediatric patients (major and minor surgeries) were enrolled.
2.4 Inclusion criteria
All surgical pediatric patients are included in this study.
2.5 Exclusion criteria
No exclusion criteria
3. Method
- Hundred patients (73 males and 27 females) were admitted to the pediatric surgery clinic to evaluate their cases and reserving dates for unit admission.
- At the appointed date the patient was asked to come with complete blood picture test.
- Patients were either admitted directly to the operation room on the day of arrivals according to a previously prepared list or they admitted to the ward unit till the day of operation which was on from 24-72 hours after arrivals.
- After the operation patients were either sent again to the ward or to the ICU according to their cases.
- Then patients were discharged from the hospital with a card of following contains the diagnosis, operation name, date of discharge, prescribed medication after discharge and assigned date of following.
-
Data in this study is classified into several classes {illustrated as
Data sheets (1-5)}:
- Patient demographic data: age, sex, weight.
- Clinical data: diagnosis, medical history, past history, family history, operation history.
- Operation type is determined.
- Risk Factors are reported for each patient.
- Medicines that are prescribed for each patient are reviewed for the correct dose, proper prescription, and interactions.
- Data were tabulated to go through statistical tests. Tests used were chi square test and 95% confidence interval.
4. Results and Discussion
A total of 100 patients were enrolled in the work. Patients are consisted of 66 (66%) infants (0-24 months), and 34 (34%) children (more than 24 months). The mean age is 27.52 ± 35.989.
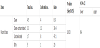
As shown in table 1 male patients are 73 (73%) and the female patients are 27 (27%).19(26%) male patients had acquired surgical site infection and 7(25.9%) female patients got surgical site infection. The previous results were in compliance with those found by Ahmed M. et al. [7] where males were more prone to surgical site infections than females. On the contrary of that was found by Afifi I. et al. [8] as the infection rate is almost similar.
By using Chi square test and 95% confidence interval in the statistical analysis we found the following:
In this study there are 60 (60%) major operations and 40 (40%) minor operations. 23(38.3) patients had major operation got surgical site infection and 3(7.5%) patients had minor operations got surgical site infection. Using Chi square test shows that there is a relationship between operation type and getting surgical site infection. As the P value = 0.001.
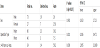
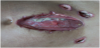
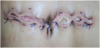
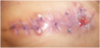
Operation type is considered as a risk factor of getting SSI. 95% confidence interval is (0.036- 0.472) as shown in table 1. Twenty six patients out of the 100 cases had acquired surgical site infections (26%) -photos of some infections (Figures 1-3). In this study a total 100 patients had undergone different types of surgery in the pediatric hospital. This percentage is considered a high percentage when it is compared with Ahmed M. et al. [7], Hafez S. et al. [9] and Petrosillo N. et al. [10]. It is worthy to mention that the results obtained by Afifi I. et al. [8] were comparable.
Differences in the rate of infection may be attributed to difference of the hospital population, underlying diseases. Differences in clinical procedures and the extent of infection control measures, difference in the hospitals environment. It can also be attributed to the high rate which resulted in this study to that the study is done in a teaching university hospital to which complex surgical cases are referred [8].
Table 2 illustrates wound class data that result in 4(8.9%) of the clean wound class, 13(39.4%) of the clean contaminated wound class, 8(47.1%) of the contaminated wound class, and 1(20%) of the dirty wound class got surgical site infections. Using Chi square test shows that there is a relationship between wound class and getting surgical site infection. As the P value = 0.003.
From the results presented it was apparent that by applying the wound class analysis 4(8.9%) were of the clean wound class, 13(39.4%) were of the clean contaminated, 8(47.1%) were of the contaminated wound class and 1(20%) were of the dirty wound class have acquired surgical site infection. The previously mentioned results were in agreement with Ahmed M. et al. [7] where clean surgical cases were 7.2% and amongst clean-contaminated cases were19.4% and with Wassef M. , et al [12] where 8.2% clean wounds, 13.8% clean contaminated and 10.1% contaminated wound cases.
On the contrary, the results obtained by Khan M. et al [11] showed that 4.88% were clean cases, 8.39% were clean contaminated cases, and 20.45% were contaminated or dirty cases.
Postoperative infections after clean procedures are most probably caused by bacteria that are part of the skin flora; exogenous sources may also be a factor, such as infected or colonized healthcare workers, the operating room environment or instruments [13]. On evaluation of the hospital adherence to the international guidelines it was found that 100 cases their prophylaxis antibiotic regimens had not adhere to the hospital guidelines.
After studying the hospital guidelines for the prophylaxis of surgical site infections the following appeared:
- The guidelines ignore the definition of prophylactic antibiotic as It should be given only pre operative before the incision by half an hour and if the duration of surgery exceeds the half life of the given drug the anesthesiologist should give another shot during the operation time.
- The prophylactic antibiotic should be discontinued within 24 hours postoperatively.
- The guidelines also ignores the determination of cephalosporins generation as the used generations in the hospital are third and fourth generation which definitely increases the resistance.
About the adherence of international guidelines shown in (tables 3, 4) we found that there was completely ignorance to those guidelines, which may be the cause the high incidence that was reported of surgical site infections in this study.
The obviously appeared SSI risk factor in this study was the more than 48 hours preoperative hospitalization. There are 24 patients had this risk factor. 10(41.7%) of patients who have risk factor have not got surgical site infection. 14(58.3%) of patients who have risk factor have got surgical site infection.
From the highly significant P value we can assure that, there is a relationship between presence of risk factors and getting surgical site infection.” Also from the 95% confidence interval we can conclude that staying more than 48 hours pre-operative in hospital is considered as a risk factor for developing surgical site infection, which is comparable to the result of Hafez S. et al. [9] (p value 0.007).
5. Conclusion
From the previously discussed study results we can conclude that; there is a high surgical site infection rate in the hospital when compared with the world wide rates or previously published researches outside Egypt.
High rates of infection may be referred to the low hygienic procedures applied during surgical operations. To minimize these rates the hospital is recommended to establish a clinical pharmacy department in the hospital with effective apparent roles and authorities, apply the international guideline in prophylactic antibiotic regimen in drug choice, drug dose and timing of injection. Infection Control team in the hospital must have an effective role in this mission. Physicians, Pharmacists, and nurses are recommended to assure the completely adherence to the roles published by the WHO.