Introduction
The International Nursing Council defines nursing as a profession where people work for the promotion of health and a safe environment, prevention of illness, and collaborative care of individuals, sick or well, in all settings [2]. This promotion of health and prevention from illness also significantly improves patients’ quality of life, knowledge of disease, and self-care practices [3, 4]. To perform such an important role in the health care system and in the lives of people who seek care, the nursing discipline requires significant rigor, quality, and excellence in the programmes with which it prepares its workforce of professional, dedicated, and competent nurses. Both the theory and the clinical component of nursing education allow students to achieve all the essential clinical competencies during their supervised clinicals which enable them to provide safe and competent care to the patients under their care [5]. This combination of theoretical nursing education with clinical practices provides personal and professional growth to students to make them eligible to contribute their knowledge and skills to society.
Nursing educators, specifically clinical educators, including faculty members and clinical preceptors, serve as gatekeepers in the nursing profession due to their responsibilities for teaching, supervising, and evaluating nursing students [6, 7]. Hence, clinical nursing educators need to excel both in the skills of teaching as well as in evaluating nursing students, to achieve the purpose of producing competent and quality nurse professionals [8].
Clinical educators have long been developing and improving their strategies to evaluate students’ performance by using different tools, such as formative and summative clinical evaluation, objective structured clinical examinations, and clinical integrated maps [9, 10]. These evaluation strategies help educators ensure extensive evaluation of students' clinical performance and correctly identify those who perform at less than average or inadequate levels.
However, despite comprehensive understanding of the evaluation process and having strategized evaluation with different evidenced based techniques, nurse educators find it difficult to identify and report students performing at low levels or those failing to achieve the minimum passing requirements. Moreover, some clinical instructors find it challenging to determine whether to fail students who display unsatisfactory practices in the clinical areas. The concept of being indecisive and allocating pass grades to nursing students who do not display satisfactory clinical practice is defined in literature as failure to fail [7].
There are multiple reasons for under-reporting unsatisfactory students, such as faculty members may face difficulty while interpreting the unsatisfactory behaviours of students, or they may have a different interpretation of clinical evaluation rubrics [11]. Tthe reluctance of faculty members in assigning failing grades to unsatisfactory students could also be due to lack of institutional support, which decreases clinical educators’ level of confidence and creates moral and ethical dilemmas [11, 12]. Furthermore, time constraints become hurdles for clinical faculty members in working with such students due to increased workload and other commitments such as administrative duties, academic responsibilities and mentorship roles [13]. Hence, for various reasons, they allow students to pass clinical courses when their competency is questionable.
Some studies have explored the perceptions of clinical preceptors and faculty members regarding the failure to fail students in nursing programs [14]. Others have examined the views of nursing students on the learning environment during clinical placements [15, 16]. However, there is limited literature available that explains the phenomenon of failure to fail within the Pakistani context.
Internationally, some studies have reported multiple factors influencing the decision of assessors while assigning grades to students in their clinical courses, which include, lack of institutional support, fear of receiving a poor evaluation from students, increased workload, and time consumption [14, 17, 18]. In Pakistan, some studies have identified students’ perceptions regarding teaching- learning strategies in the clinical environment [16, 19, 20]. However, as per the researcher’s knowledge, in the nursing education system of Pakistan, the phenomenon of failure to fail and the perceptions and experiences of clinical educators on this issue have not been studied yet. Hence, there was a need to examine if the issue of failure to fail nursing students in their clinical courses exists in the nursing educational system of Pakistan and if it exists then what are its reasons and how it can be corrected. The study aimed to identify the challenges local clinical educators face in assigning failing grades to students and examine how these challenges perpetuate a culture of failure to fail within nursing education, contributing valuable insights to improving assessment practices and ensuring the development of competent nursing professionals.
The study research question is:
What are the perceptions and experiences of clinical preceptors and faculty members about failure to fail undergraduate nursing students displaying unsatisfactory practices in their clinical at a private school of nursing and midwifery in Karachi, Pakistan?
Methodology
The qualitative descriptive-exploratory design was chosen as it is ideal for exploring subjective experiences, beliefs, and attitudes, aligning with this study's aim. This approach effectively addresses the complex and sensitive issue of "failure to fail" in nursing education by offering flexibility and depth in capturing participants' perspectives. It is particularly suited for context-specific research like this study in Karachi, Pakistan [21].
The study was conducted at the private nursing school Karachi, Pakistan. The purposive sampling technique was utilized to identify participants who could provide detailed information about the concept.
A total of 12 participants were recruited in the study, based on data saturation. The data collection was stopped after meaningful information had been attained [22, 23]. All full-time and part-time nursing faculty members and clinical preceptors who possessed at least one year of experience of teaching one or more clinical courses to undergraduate nursing students and gave voluntary verbal and written consent to participate in the study were included.
After obtaining approval from the Ethical Review Committee of the institution (ERC), a list of clinical preceptors and faculty members was obtained from the clinical practice office of the private nursing school. Subsequently, the clinical preceptors and faculty members who fulfilled the study inclusion criteria, were approached through electronic mails, and an invitation letter was given by the researcher. The study was conducted, after approval from the (ERC), from January 2020 to September 2020. The data was collected through face to face semi-structured in-depth interviews.
An interview guide was developed by the researcher. The interview guide was developed based on the study's research question, focusing on the perceptions of faculty and clinical preceptors regarding failure to fail students. It included open-ended questions designed to explore participants' experiences and views. The guide was structured with opening questions, core questions, probing questions, and concluding questions to gather comprehensive insights. The guide was refined using existing literature [21, 24] and pilot testing to ensure clarity and relevance, with ethical considerations ensuring neutral, non- judgmental questions. Additionally, a demographic questionnaire also developed which helped in ensuring a diverse selection of participants, in order to have rich data on the phenomenon of interest. The researcher conducted in-depth interviews, and each interview lasted for 60-70 minutes. These in-depth interviews allowed faculty members and clinical preceptors to discuss and reflect on the phenomenon of interest. The interviews were conducted in English and were audio-recorded for analysis. Simultaneously, note-taking was maintained to capture non-verbal clues that could not be revealed in audio recordings. Interviews were conducted in the offices of the faculty members/clinical preceptors, and timings were decided as per the feasibility of the researcher and participants to ensure their availability for the interviews. Initially, the interview guide was pilot tested on two faculty members from the sample to ensure that questions were clear, logical, and understandable by the participants. These pilot interviews were included in data analysis and the sample size of the study.
To maintain anonymity throughout the study, each participant was assigned an identification number. Privacy and confidentiality were upheld by securing hard copies of transcripts and consent forms in a locked cupboard, while soft copies were stored in password-protected files accessible only to the researcher, supervisor, co-supervisor, and committee members.
In accordance with institutional policy, all audiotaped files will be discarded. Autonomy was respected by ensuring participants’ voluntary involvement and the protection of their personal information.
Data analysis
The method of data analysis employed in this study was content analysis, following Creswell’s [1] guidelines. Content analysis was chosen because it provides a structured approach to interpreting and categorizing qualitative data, allowing for a deeper understanding of patterns and themes. During the interviews, data was audio-recorded, and the recordings were then transcribed and organized as part of the data analysis process.
To ensure anonymity and confidentiality, each participant was assigned a unique identification number (ID#). This helped in maintaining privacy throughout the study. The interviews were transcribed in English, and the transcriptions were stored as text- based data in a Word document. Since the interviews were conducted in English, there was no need for translation. Each transcription was carefully read multiple times to identify key concepts and ensure a comprehensive understanding of the data.
The transcriptions were divided into five categories: identification numbers of participants, their transcriptions, codes, categories, and themes. Data with similar meanings were grouped under common codes. These codes were then analyzed and merged into broader categories, allowing for a clearer understanding of the main findings. Each category was supported by relevant participant quotes extracted from the transcriptions, providing concrete evidence for the analysis.
Following this, similar categories were combined to form overarching themes. These themes were analyzed in relation to recent literature to ensure the findings were grounded in existing research. To enhance the robustness of the analysis, the supervisor, co- supervisor, and committee members were consulted for their input, particularly in comparing the data with the literature and drawing meaningful interpretations. Finally, the data was visually represented in a diagrammatic format, which helped in effectively illustrating the study's findings.
Results
The study included 12 participants, consisting of faculty members who teach both theoretical and clinical courses, as well as clinical preceptors who focus on teaching clinical practice. Participants, teaching in different undergraduate programmes, and several clinical courses, in different years, were recruited to get diverse data.
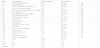
The overall descriptive analysis of the demographic data of the participants is presented in table 1.
Themes and categories from the qualitative study findings is presented in table 2.
Theme two-category one (Evaluation tool is unclear):
Seven of the 12 participants expressed that observing and evaluating in the clinical setting is subjective. Further, students are evaluated on several clinical and professional skills, based on pass or fail. This criterion of evaluation creates subjectivity and biasness among clinical educators. As one of the participants stated:
“First of all it is very difficult to fail the student in the clinical area because it is highly subjective” (ID#015).
This quotation reflects the participant's belief that assessing students in the clinical setting is challenging due to the subjective nature of evaluations. The participant suggests that clinical assessments are influenced by personal judgment, making it difficult to assign failing grades.
Furthermore, some participants also shared the need for and importance of having specific rubrics for evaluating students’ clinical performances. Unavailability of such rubrics creates difficulty in deciding and assigning failing grades to students. As one clinical educator reported:
The clinical evaluation criteria have only four components; the Likert, as pass, fail, not applicable, and incomplete. So, the proper rubric that what we think is pass and what we think is fail, incomplete, and not applicable is not being defined. Currently, there is no rubric, it’s a faculty’s decision, that’s the limitation that why we are not failing. There is no black and white thing written, there is no rubric to it. (ID#011)
Theme two-category two ( Nursing is not the first choice of students ):
Participants noted that nursing is often seen as a last-choice career, with few students choosing it due to its lower societal status. One participant highlighted this as a challenge for clinical educators, who, as expressed by participant ID #004, are reluctant to fail students "because they fear it will discourage people from entering the profession."
Theme three-category one (Feeling of guilt):
Many study participants cited a feeling of guilt in the process of failing an unsatisfactory student in their clinical placements. A participant expressed a feeling of guilt at not provided proper support to enhance a student’s capability. This let to hesitation in assigning a failing grade to the students in the clinical settings.
There are two things that I will face, first is my personal feeling, because if he or she is going to fail at the end of our clinical then for what purpose was I there? Like you know I will feel guilty about it, that, why did not I make that particular student capable to pass at the end of the duration or the clinical rotation? (ID # 009)
Another participant stated:
“For me if somebody is failing means I have failed” (ID#007)
Theme three-category two (Fear of getting bad evaluation from students):
Some of the study participants stated that they might get negative evaluation from students if they fail them. Clinical educators may not consider to fail students in clinical settings to prevent harming their good reputation among student body which may help them to get nominated for best teacher award. Moreover, the participants also mentioned that those clinical educators who evaluated the students strictly were considered as strict teachers and were disliked by most of the students. As one faculty member reported:
If we at all fail, and this happens very commonly, very commonly it happens that Oh we are the most disliked faculty. She likes to fail, she doesn’t like me that’s why, all those kinds of statements we hear from the students. In our evaluations, you know, we get to know, so clearly, that we are so bad, the worst faculty in the world (making sad face). (ID#006)
Another participant, while stating her feelings, said:
So I become you know someone highlighted, this teacher is very strict and students avoid that particular teacher. So that’s what I personally faced and I was feeling very bad. Because I am very strict with my students, with the passage of time I got that feedback that I should be a bit lenient, and that leniency was at the end meant that I should not be very strict in assessing. (ID # 007)
Theme three-category three (Family reaction on failing their children):
The participants also identified that failing a student in a clinical placement can lead to significant emotional and financial burdens on students and their families. As one faculty member pointed out,
Students probably, you know, will get punishments when they go home. If they say I failed the exam, how will the mother react, how will the father react? How will the in-laws react? How will the friends react? So that is emotionally challenging and, after all, obviously, the longer the time the student is there in the institution the more finance is required. (ID#006)
Theme three-category four (Students’ own reactions on Failure):
A few of the participants found it difficult to fail unsatisfactory students because of the students’ reactions. Clinical educators face disrespect as students’ response to failing them in the clinical areas. As depicted in conversation with one of the participants:
“The hatred I can see in his eyes. He wishes every faculty, but he does not wish me (2 sec. pause). He is right in a way that I have delayed his convocation for a year, otherwise, you become blind and go away” (ID#008).
Additionally, a participant who was trying to help a student achieve clinical learning outcomes, verbalized about the threatening attitude of the student.
A student was not performing well, and I gave him feedback, but he was not changing, so I put him on a learning plan (pointing towards herself). The student perceived this negatively, but it is like, you know, in response I received nonverbal clues, I was very fearful and very anxious. (ID# 014)
Discussion
The participants in the research study felt that due to inappropriate evaluation tools they faced difficulty in evaluating unsatisfactory students. They identified subjectivity in the evaluation tools while evaluating students on clinical placements [25]. Moreover, the study participants found that subjectivity in the evaluation forms increases the risk of evaluators’ interpretation, resulting in, under-reporting of correct observations of unsatisfactory students. This can be related to the finding of DeBrew and Lewallen [26], that clinical educators found that the number of times the students had been evaluated was less defined in the evaluation tools, which made it further challenging for evaluators to assess the unsatisfactory behaviours of students. Further, the participants articulated that there was no detailed rubric for evaluating clinical performances of students, so, the clinical educators were unable to quantify students’ performances. Likewise, findings by Helminen et al. [27] show that evaluators feel confident while using clear assessment tools for assessing students on clinical, and this also reduces the risk of subjectivity. This suggests that unclear evaluation processes and non-availability of a clear specific rubric makes it challenging for assessors to rate students’ performances, which develops ambiguity in assessing unsatisfactory students.
Considering the perceived views of society, regarding nursing as a less privileged profession, clinical educators were reluctant in assigning a failing grade to unsatisfactory students due to the fear that highly stringent evaluation and failing more students may result in further decrease in number of students selecting in this profession. Whereas some participants identified that students considered nursing as a last choice for higher studies and when students with unsatisfactory behaviours are promoted in the programme, this can promote a negative image of the profession. As per the researcher’s knowledge, these findings are unique for the phenomenon of failing to fail nursing students in the clinical courses. This finding is relevant to the context, because, still, nursing is not considered as a preferred profession by students. Hence, this is a new knowledge added to the literature, by this study.
Furthermore, consistent with the findings of Luhanga et al. [5], clinical evaluators faced difficulty in communicating failing grades to students, based on the year of the study programme. The participants mentioned that communicating failing grades to students in the initial year of the programme was too early hence they prefer, giving students constructive feedback and time to improve their competence in clinical areas in future. However, some participants articulated that in the initial years students are assessed on basic skills and knowledge, and if they are unable to show the required competency level, then faculty members must fail such students. Studies have mentioned that dealing with unsatisfactory students and assigning failing grades in the early year of the programme is important to identify suitable students for the programme [5, 6, 28].
On the other hand, study participants also mentioned that they lacked the courage to communicate the failing grade to unsatisfactory students in the final year of the programme. The same has been identified by Hunt et al. [23], in that participants found it difficult to recognize and to take the responsibility of failing unsatisfactory students in the final years of the programme, when they are near to their graduation. In correspondence with this, in the findings of Docherty and Dieckmann [29], the participants also highlighted that the clinical evaluation process was not specified according to the year of the programme, so it made it difficult for the assessors to assign failing grades, specifically to the standards in their final year of study [29]. On the other hand, clinical educators should realize that students in their final year are near to the completion of their studies and are expected to have advanced skills and knowledge of clinical experiences to which they were exposed [17]. This suggests that while students are assessed in the initial years of the programme on basic skills, in advanced years they are evaluated on more complex concepts. Thus, while assessing students regardless of the year of the programme, it is essential to identify unsatisfactory students and take needful steps to make them more competitive for their profession.
While discussing the emotional challenges, the findings of this study are consistent with the results of the study conducted by Black, Curzio, and Terry [30] which identified that clinical educators felt self-responsible, had a sense of guilt, and they questioned their competencies when deciding to fail students in their clinical placements. Moreover, this present study also identified that participants had the perception of self-failure, and they doubted their own judgment in assessing and supporting students in clinical placements. This stance is supported by several studies, in which assessors had a feeling of personal failure, guilt, and self-blame while failing unsatisfactory students [30-32], 28, 17].
Moreover, the clinical educators in this study mentioned that they had a fear of receiving a bad evaluation from students, if they did not pass them in their clinical settings. In line with Pratt et al. [32], this study also found that clinical educators had a fear of getting negative ratings from students, which led them to pass students instead of standing firmly on their decision of failing them. This was consistent with the findings of Couper [33], where the participants felt bad for students while assigning failing grades to them and had a fear of getting a bad evaluation from students. Although, it was not often mentioned in the present study, literature has identified that many of the clinical faculty members had a close teacher student relationship with students, thus they believed that failing students may create an unhealthy relationship with them in the future [28]. This suggest that clinical educators considering negative effects on self-evaluation do not attempt to fail students with unsatisfactory performance according to their knowledge and competency. Hence, this is an eye opener for the system, to improve their evaluation practices for producing competent nurses. As per the researcher’s knowledge, the significant finding in this study was that faculty members considered the financial burden upon students and their families as a preventive factor and as a consequence, so, they do not declare failing grades to students on their unsatisfactory practices. Additionally, this study reported a unique finding that clinical educators were also unable to fail students because, as a result of failure, they would get punishments at home.
Conclusion
The study found that the decision to fail nursing students in the clinical setting is challenging. Despite recognizing unsatisfactory practices, educators face barriers in assigning failing grades due to societal perceptions and the fear of discouraging students. To address this, it is recommended that nursing programs provide faculty with training on objective, evidence-based assessments and clear guidelines for making difficult decisions. Strengthening the clinical evaluation process will ensure fairer assessments and help produce more competent nurses. Improving clinical evaluations will enhance nursing education and address the profession's challenges, ensuring that only adequately prepared students enter the workforce.
Strengths and Limitations
The strengths of this study include its novelty, as it is the first of its kind in Pakistan to explore the perceptions and experiences of faculty members and clinical preceptors regarding the challenge of failing nursing students in clinical courses. It also identifies key areas for improvement in the clinical evaluation system to help produce competent nurses. Additionally, the use of in-depth interviews conducted by the primary researcher provided valuable insights into the phenomenon under investigation.
However, the study also has limitations. It was conducted in only one nursing educational institution, which means the findings cannot be generalized to other nursing programs or settings in Pakistan.
Competing Interests
The author have no conflicts of interest to declare that are relevant to the content of this article.
Authors Contributions
The primary author conducted the research, analyzed data, and drafted the manuscript. Dr. Farhana Madhani and Ms. Shirin Rahim provided critical feedback and guidance throughout the process. Dr. Rubina Barolia offered valuable insights and supervision. All contributors approved the final manuscript.
Acknowledgments
The authors extend their gratitude to all the participants who took part in the study.