Research Background
The Basic Law on Cancer Control, which came into effect in Japan in 2006, shows the basic philosophy of establishing a system to provide cancer medicine so that the treatment method of cancer is selected with full respect for the intention of the cancer patient according to the situation in which the cancer patient is placed [1]. Furthermore, in the 3rd Basic Plan for Promoting Cancer Control in 2012, it is necessary to enhance the system for providing home medical care and nursing care, including home palliative care, so that patients can choose to recuperate and live in their familiar homes and communities [2]. These have shown the importance of decision support for cancer patients in order to be themselves until the end. Although cancer is not the only disease that is reaching its end, in recent years, "Advance Care Planning: ACP" has been attracting attention as one of the methods of decision support with an eye on the end of life.
In 2015, the International Delphi Panel was held, and problems such as the definition of ACP and the contents of ACP practice were examined by ACP clinicians and researchers. In this report, it is shown that it is important to obtain medical care and endeavour in line with the patient's own values [3].
Until now, the existence of problems such as immaturity and lack of confidence in the knowledge and technology of end-of-life care of ward nurses has been discussed [4]. In addition, it has been pointed out that the reluctance attitude of ward nurses to home care of terminally ill patients and problems such as home care not being conscious as an option [5]. In particular, there are reports that ward nurses in acute hospitals are finding it difficult to support decision- making in the daily life of performing complicated tasks while looking after surgical patients and severe patients [6]. In general wards, care is often experienced in parallel with the assistance of medical care such as examination and treatment of patients and the aid of daily life. In end- of-life care in general wards, there is also a point on the current situation of "not clearly focusing on spiritual pain" and "pain management cannot be said from the viewpoint of total pane" [7].
End-of-life care is not only carried out at specific facilities such as hospice and palliative care wards, but also in general wards. However, until now, there are few studies that have investigated the present state of advanced care planning in end-of-life care of ward nurses based on the actual situation. Therefore, it was considered that it was necessary to clarify the present state of the ward nurse for advanced care planning for the decision support of the terminal stage. The purpose of this study is to clarify the present state of ACP implementation in end-of-life care of ward nurses. Furthermore, we will examine the problems for the implementation of ACP to improve the quality of end-of-life care in general wards.
Research Methodology
Research design
Cross-sectional research by questionnaire survey
Target
This paper is aimed at general ward nurses in hospitals that provide terminal care in regional cities of Japan, A, B, and C prefectures.
Survey period
The survey period was from April 2020 to September 2020.
Survey items
The survey items were about 1) basic attributes of individuals, 2) ACP practice status, and 2) question items were prepared with reference to the survey for the Ministry of Health, Labour and Welfare [8] to make it a material for considering medical care at the final stage of life.
1) Basic attributes of individuals Overview of the target audience
As basic attributes, we asked about age, gender, number of years of nurse experience, training on decision-making, frequency of involvement with terminally ill patients, etc.
2) ACP practice status
Regarding the status of ACP practice, we asked about the existence of ACP practice, the degree of discussions on medical care and medical treatment, the experience of confirming the place to reach the end, whether it is recommended to use writing in advance in case it is impossible to make decisions, and when to confirm who can make proxy decisions.
Survey methodology
We explained the purpose of this study in a document to each hospital manager, and started the investigation after obtaining the consent of research cooperation. We asked the hospital manager who had obtained consent to request the investigation to the survey subject, to distribute the survey manual, questionnaire, and return envelope. The method was used as a mailing method of anonymous self-written questionnaire.
Analysis method
Descriptive statistics were calculated for each question item of basic attributes and ACP practice status of individuals. In addition, the correlation coefficient was calculated for the relation between the characteristics of the subject and the ACP practice situation. This test used the rank correlation coefficient of Spearman as a nonparametric method. The statistical software SPSS Statistics ver25 was used for the analysis.
Ethical considerations
The survey form was anonymous and no individual was identified. This research was explained in a document, and the answer was added that it was optional, and it was possible to cooperate with this research by free intention, and it was agreed by the return of the investigation form. It was carried out with the approval of the A University Ethics Review Committee (approval number: 015 dai, 30 hei).
Operational definitions of terms
ACP: A process to help all adults, regardless of their age or health condition, understand and share their values, life goals, or their intentions and choices regarding medical care and recuperation [3]. General wards: The hospital beds, including psychopath beds, infectious disease beds, tuberculosis beds, and beds other than recuperation beds [9].
Result
Recovery rate
There were 5 hospitals that were requested to 8 hospitals and obtained research cooperation. The target hospital was a general hospital with 300 to 500 beds, and it was a hospital responsible for core medical care in the region. Responses were obtained from 372 general ward nurses for 500 nurses. The recovery rate was 74.4%. We analyzed 369 responses except those with incomplete answers and extreme biases. The effective response rate was 73.8%.
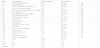
Characteristics of the target person (Table 1)
The average age was 40.4 ± 10.7-year-old, 15 males, and 354 females. The most years of nurses were 72 (19.5%) in 1-5 years, followed by 63 (17.1%) in 11-15 years, 59 (16.0%) in 16-20 years, and 48 (13.0%) in 21-25 years. The most common awareness of ACP was "vaguely understood" at 164 (44.4%), followed by 98 (26.6%) who had never heard of it. The most common attitude toward ACP was 217 (58.8%). 270 people (73.2) had not taken. In addition, 211 (57.2%) felt difficulty in confirming intentions related to end-of-life medical care and care.
Status of ACP Practice (Table 2)
99 (26.8%) of patients in the final stages of life said they practiced ACP, and 270 said they did not practice it ( 270 ) 73.2% of respondents answered that they were "doing enough" to discuss medical care and medical treatment, and 180 (48.8%) answered that they were doing so, and 56.4% said they were doing so. 235 (63.7%) answered that they had done so to confirm the place where the end of the year was reached. 245 (66.4%) answered that they had indicated their support for the selection of the final place.
Relationship between characteristics of the target audience and the status of ACP practice (Table 3)
The following results were obtained on the relationship between the characteristics of the subject, the presence or absence of ACP practice, the degree of discussion, and the usage of the advance instruction center. Regarding "recognition of ACP", there was a weak positive correlation between "practice of ACP for the subject in the final stage of life", "confirmation of how to take care and the place where the end will come", and "support for the selection of the place to reach the end". Regarding the attitude toward ACP, there was a weak positive correlation between "the practice of ACP for the subject in the final stage of life", "discussions on medical care and medical treatment", "confirmation of how to take care and the place to reach the end", and "support for the selection of the place to reach the end". In addition, there was a weak positive correlation between "practice of ACP for the subject person in the final stage of life" and "discussion about medical care and medical treatment" in "training on decision support".
Consideration
Relationship between the characteristics of the target audience and the ACP practice situation
In this study, there was a weak correlation between the characteristics of ward nurses and the ACP practice situation, but not a significant correlation. However, it was shown that "awareness of ACP", "attitude toward ACP" and "training on decision support" in the characteristics have a weak correlation with the ACP practice situation, and that working on these leads to the promotion of ACP practice.
Takenouchi describes the necessity of decision support and ACP from diagnosis to end of life in order to improve the quality of decision support for cancer patients [10]. In addition, it has been pointed out that the patient is hospitalized on the occasion of some kind of medical condition change, but the situation that the prognosis is not so imminent but there is a change in the condition is easy to start ACP [7]. However, it has become clear that general ward nurses are not supported for decision-making in order to reach a satisfactory end to patients and their families in busy daily work. More than 60% of the respondents confirmed "how to take care and confirm the place where the end of the year", and more than 60% showed support for the selection, but it became clear that the actual situation felt difficult.
It was not possible to see the insufficient educational opportunities such as training which becomes the base for the nurse to carry out ACP and the lack of preparation of explanatory materials. In the future, it is a problem to construct an organizational support system for ACP practice.
The limits of This Study and Future Issues
Since the question items set in this study are limited to items set with reference to the previous research, there is a possibility that there are other answers and distributions. Therefore, there is a limit to the generalization of this study. In the future, it is a problem to expand the target facility and target person, and to conduct the investigation which can catch the whole picture of the subject who added the interview investigation and the free description.
Conclusion
In the busy daily work, it became clear that the lack of educational opportunities such as training and preparation of explanatory materials became clear, which is the basis for ward nurses to carry out ACP in close contact with terminally ill patients.
Acknowledgments
I would like to express my deepest gratitude to the administrators and target users of the target hospitals for their cooperation in this research.
Competing Interests
The author declare that there is no competing interests regarding the publication of this article.
References
- Ministry of Health, Labour and Welfare (2006): Basic Act on Cancer Control, Retrieved on August 12, 2020). View
- Cancer and Disease Control Division, Health Bureau, Ministry of Health, Labour and Welfare (2017): Partial revision of the Basic Law on Cancer Control and the status of examination of the 3rd Basic Plan for Promoting Cancer Countermeasures, Retrieved on August 12, 2020). View
- Sudore RL, Lum HD, You JJ, Hanson LC, Meier DE, et al. (2017) Defining advance care planning for adults: a consensus definition from a multidisciplinary delphi panel. J Pain Symptom Manage 53: 821-32. View
- Sasahara T, Miyashita M, Kawa M, Kazuma K (2003) Difficulties encountered by nurses in the care of terminally ill cancer patients in general hospitals in Japan. Palliat Med 17: 520-526. View
- Sato M, Hirose Y, Asai M (2011) Problems in support for transition to home palliative care to end-of-life cancer patients by staff nurses From the recognition of nurses in charge of community medical cooperation. Chiba Health and Medical Bulletin 2: 63-69.
- Toyama H, Mihara K (2008) Roles and Problems of Discharge Coordinator Nurses: Looking back on the current state of discharge adjustment in acute hospitals. Medical Journal of Shimane Central Hospital 33: 26-28.
- Nakagi S, Eguchi H (2020) Literature review on the present state and problems of end-of-life care in acute wards. Sanyo Ronso 27: 33-42.
- Ministry of Health, Labour and Welfare (2016) Survey on medical care in the final stage of life, Retrived on December 12, 2019)
- Ministry of Health, Labour and Welfare (2007) on the medical facility system, Retrived on December 12, 2019). View
- Takenouchi S (2015) Improving the quality of decision support for cancer patients- "Decision support" and "advanced care planning" from diagnosis to the end of life, nursing management 25: 125-133.