Introduction and Background
Professional nursing practice is a vital component of undergraduate nursing programs, allowing students to apply their theoretical knowledge in real-world settings [1, 2]. Clinical nurse educators play a critical role in guiding and assessing nursing students during their clinical rotations, facilitating the development of necessary knowledge, skills, and competencies for future healthcare professionals [3, 4].
In Canada, nurses fulfilling entry-to-practice standards by instructing and supervising students across various practice courses are commonly called clinical instructors. Typically, they are part- time employees of hospitals who teach professional practice courses at universities for a semester [5]. The literature emphasizes that clinical instructors must have expertise in the practice environment, curriculum, and professional skills, support students, encourage critical thinking, and uphold teaching standards [1, 6]. However, a debate surrounds the idea that while nurses excel in patient care and hands-on support for students, not all possess the requisite educational expertise [7]. Additionally, many clinical instructors are hired without sufficient teaching experience and their part-time status in the role may leave them feeling unprepared for the work [8-11]. Benner [13] also asserted that novice instructors may experience a lack of confidence, stress, and anxiety due to inadequate experience and exposure.
Nursing education research primarily focuses on defining the general roles and responsibilities of clinical instructors. These studies emphasize the critical role of clinical instructors in guiding students' learning experiences, providing constructive feedback, and assessing their clinical competencies [13, 14]. Other research explores faculty and student perspectives on clinical instructor traits affecting student progress. For example, Al- husban et al. [15] studied nursing students' perceptions of clinical instructors' caring behaviours. Similarly, other studies identified positive behaviours for effective clinical instruction [16-18] and behaviours hindering student progress [19, 20]. Additionally, some studies examine issues related to evaluating nursing students' clinical performance [21, 22].
While numerous studies have explored various aspects of clinical education and emphasized the crucial role of clinical instructors in student learning within clinical settings, limited research has examined the experiences of these instructors when it comes to facilitating and evaluating nursing students during their professional practice courses. For instance, an Australian study by Andrews and Ford [23] identified effective clinical facilitation strategies, including mentorship, feedback, and communities of practice, which bridged the theory-practice gap for nursing students during placements. Similarly, a study in Finland and Sweden [24] explored preceptors' roles in supporting nursing students, emphasizing the importance of a supportive environment for both parties. In Indonesia, a cross- sectional study [25] found that clinical instructors generally hold positive views of their role despite demographic factors influencing their teaching effectiveness. A study from Malawi [26] revealed that experienced preceptors with a Bachelor of Science in Nursing felt confident in their roles. Additionally, a qualitative study from Taiwan [27] highlighted challenges faced by clinical instructors in teaching, while an earlier study from Manitoba [28] detailed the learning process and challenges of clinical teaching for novice and expert teachers.
Despite the existing literature on the topic, studies examining the experiences of clinical instructors vary in age and scale, which limits their scope in capturing the diverse experiences of clinical instructors. Moreover, the ongoing shortage of nurses in Canada has prompted the government to allocate funding to universities to increase enrollment in nursing education and address the gap [29]. The COVID-19 pandemic has exacerbated this situation, intensifying the urgent need to strengthen the nursing workforce [30]. To meet this demand, nursing schools may need to hire more clinical instructors and adequately prepare them for their roles. Therefore, further exploring this phenomenon is crucial for enhancing students' clinical practice experiences and providing necessary support resources to clinical instructors. The present study aims to delve deeper into the experiences of clinical instructors in facilitating and evaluating students' performance in a professional practice course at an Ontario university.
Methodology
Study design
The study employed an interpretive descriptive research approach, focusing on collecting and analyzing data to capture the experiences of clinical instructors in the clinical context of applied health disciplines [31]. This methodology, aligned with constructivist and naturalistic inquiry, offers valuable insight into practical issues clinical instructors face and informs the development of strategies to address their needs [31]. Two primary research questions guided the study:
1. What are the experiences of clinical instructors in facilitating and evaluating nursing students in a
professional practice course?
2. How do clinical instructors recommend enhancing clinical teaching, facilitation
skills, and practice?
Sampling and data collection
The study was conducted from 2022 to 2023 and utilized purposive sampling. Eligible clinical instructors in the nursing program, who had a minimum of 6 months of experience in clinical teaching, were invited to participate via email. This approach aimed to gather diverse perspectives and insights into the experiences and challenges encountered by clinical instructors at various stages of their careers. Semi-structured interviews were conducted in person, via telephone, or through virtual platforms like MS Teams or Zoom, adhering to COVID-19 guidelines. Before each session, participants received a verbal explanation of the study objectives and the right to withdraw and were encouraged to ask questions. Twelve clinical instructors provided written consent, and interviews lasted 60 to 90 minutes, guided by a semi-structured interview guide and audio recorded (Appendix A). The interviews were transcribed with identifying information removed, and filed notes were maintained during the interview. Ethical approval was obtained from the participating institution's Research Ethics Committee, and participants received an honorarium.
Data analysis
Each interview was digitally recorded and transcribed verbatim. An audit trail and memos were maintained on a password-protected laptop and secure server. The transcripts were carefully read word-by- word and coded to determine initial categories. An iterative process of data analysis involved repeated reading, reviewing, and refining of categories and themes reflecting experiences associated with clinical facilitation and evaluation [31]. The study followed Lincoln and Guba's credibility principles to ensure trustworthiness [32].
Findings and Discussion
Characteristics of the participants
All twelve participants in this study were female, with an average of 3.2 years of experience working as clinical instructors, ranging from 1 year to 9 years. Regarding educational background, most participants (n=9, 75%) held a Bachelor of Science in Nursing degree, while the remaining participants had obtained a Master’s degree (n=3, 25%). The average years of registered nurse experience among these participants was 4.7 years, ranging from 1 to 13 years working at the hospital or in public health settings. Four participants (33%) have a full time work elsewhere. All participants have completed additional diplomas and certifications such as Advanced Cardiac Life Support, Pediatric Advanced Life Support, Emergency Nursing Pediatric Course, Oncology, Public Health, and Health Care Leadership.
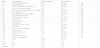
A content analysis of the data yielded insights into clinical instructors' experiences facilitating and evaluating nursing students in a professional practice course. These insights were categorized into six major themes: (a) inconsistency and uncertainty in course expectations, (b) limited understanding and experience with clinical evaluation, (c) considerations regarding failing a student in professional practice course, (d) absence of performance evaluation or feedback, (e) balancing workload and adaptation during pandemic uncertainty, and (f) inadequate instructor orientation and mentorship. Table 1 highlights the themes and sub-themes that emerged from the analysis.
Theme 1: Inconsistency and Uncertainty in Course Expectations
The clinical instructors discussed the details of their roles and their comprehension of the expectations associated with being an instructor in the professional practice course. They pointed out challenges in defining their roles and setting expectations, particularly when there is a lack of clarity on course objectives. A participant said, “…for me when I was starting out as a new clinical instructor, these objectives are very wage and …for my own … and did I deem understand these objectives, my answer is no” (Participant 3).
It becomes even more challenging when the clinical instructor is new, as they are still developing their teaching skills and struggle more with unclear course objectives and expectations. A few novice clinical instructors, who are new to their role, expressed feeling overwhelmed by the lack of clarity regarding the course objectives. One participant stated, “I am not clear on what a student can and cannot do on the clinical” (Participant 2). Participants also expressed frustration with inconsistent guidance from professors, which results in variability in teaching approaches and resources utilized. For example, a participant who taught across different years and with different professors mentioned,
I find it challenging to clearly define my role and set expectations when I am not so clear about the course objectives. There are professors who spell out everything for us, and there are others… don’t explain them [objectives] and leave them on us to figure out… It can be especially overwhelming for clinical educators who lack experience and are developing their teaching skills (Participant 10).
The clinical instructors mentioned they are expected to provide clear guidance to their students and to ensure they are meeting learning outcomes. They shared their struggle to align their teaching with varying expectations and use of various tool, leading to confusion for both themselves and their students. As one participant mentioned, “depending on the professor, sometimes I am using this clinical care sheet, sometimes I am using this... for patient research…” (Participant 4). Hence, lack of clarity hinders their ability to effectively facilitate learning and achieve the course objectives, particularly when different professors use varying methods or materials.
Literature on clinical education emphasizes the crucial need for clinical preceptors and nursing instructors to fully grasp course objectives, as they are essential for facilitating engaging learning experiences for students [33]. Additionally, Zuhroidah and colleagues [34] stress the significance of such clarity in course objectives, as it empowers instructors to offer guidance and support to students, thereby aiding them in achieving desired learning outcomes. Consequently, when instructors thoroughly align with course objectives, they can effectively tailor their teaching methods and clinical experiences to meet these goals [14].
Participants in this study stressed the significance of receiving clear guidelines from the course professors and highlighted how having the course syllabus well in advance enabled them to review and comprehend its contents. Some instructors mentioned the benefit of regular meetings with the course professor, particularly at the beginning of the term, as it helped them ease into their role and gain a deeper understanding of the course objectives. For example, one participant stated, “We have expectations to facilitate students on clinical…so having a clear understanding of the course objectives is vital for me to play my part” (Participant 7). They suggested that having a solid understanding of competencies and “a clear list of competencies or skills based on the student’s program level would be a helpful step” for instructors to follow to meet the course expectations (Participant 9).
Henderson and colleagues' [35] review emphasizes the importance of consistency and standardized methods in clinical education to enhance nursing students' learning experiences and improve the effectiveness of clinical instruction. They suggest that maintaining consistency and standardization in teaching methods, evaluation criteria, and expectations can allow students to better understand what is expected of them and how they will be evaluated. There were three clinical instructors in this study who raised the issue regarding the challenge of understanding the course expectations when the course professor is new to the course. This highlights the importance of clear communication and coordination between faculty members involved in nursing education. A participant with good numbers of clinical and teaching experience said, “You don’t know what you don’t know… if a course professor is new to the course, they really don’t know the content either, so it is hard to say what is needed…” (Participant 1). The role of the course professor in setting course expectations and aligning them with the evaluation process is crucial. Conversely, experienced professors are more likely to have a clear understanding of course expectations, making it easier for clinical instructors to align their evaluations with these expectations. As another participant said, “If it is an experience professor it is easier to know what the course expectation are and if it a novice professor, it won’t be very clear” (Participant 5).
While existing literature may not directly address this specific scenario, Kohan et al. [36], in their systematic review, emphasize the significance of collaboration and communication among faculty members in nursing education to ensure effective teaching and evaluation practices.
Additionally, providing new course professors with comprehensive orientation and training programs could alleviate some of the challenges identified by clinical instructors in the evaluation process. Further research may be needed to explore how the experience level of course professors affects the clarity of course objectives and its implications for clinical evaluation practices. Within the Canadian context, Melrose [37] stresses that clinical instructors must thoroughly understand the curriculum to teach and evaluate students effectively during their clinical rotations. The author emphasizes that clinical instructors, who are critical figures in the nursing education system, must be well-versed in the learning outcomes and content covered in the nursing curriculum. This will help them apply theoretical knowledge to clinical practice and navigate complex patient care scenarios. Future research should investigate strategies to improve clarity and consistency in course objectives for clinical instructors, particularly for novice educators.
Theme 2: Limited understanding and experience with clinical evaluation
In this study, clinical instructors shared several challenges they faced regarding the clinical evaluation processes. Many participants voiced their concerns about lacking knowledge and experience in understanding the evaluation process or comprehending the evaluation tool. One participant stated, “I am supposed to evaluate students on several competencies…but I don't feel confident completing the tool as there are too many components within each competency, and often I don’t find opportunities to assess students” (Participant 2).
Another participant with less than two years in the role said,
The evaluation tool is subjective, and it is very long… the tool touches many areas… I think it is well rounded in that way…. students either meeting or not meeting, where they are on a scale… especially things like critical thinking, some student may be meeting the objectives but at a different degree whereas sterile techniques, did they contaminate or not contaminate, well that’s easy to see, …. this is black and white. For instance, in professional development, they are meeting and sometimes they are not…I want to know what the cut-offs on the evaluation sheets are… (Participant 11).
Participants highlighted the length and complexity of the clinical evaluation tool, expressing concerns about its subjective nature. They emphasized the need for more precise, objective criteria and support for new clinical instructors to understand the tool. Wu and colleagues [38] reported that clinical instructors or preceptors unfamiliar with the assessment system can affect their ability to help students integrate theoretical knowledge with clinical practice. Variations in how they interpret competency standards also lead to inconsistency in their approach to assessment. Literature focusing on clinical education asserts that nurse educators bear the responsibility of equipping students with the necessary knowledge, skills, and attitudes to navigate the complexities of clinical practice [39, 40]. Therefore, they should have a clear understanding of the curriculum and the components they will be evaluating in their students. In addition, Burgess et al. [41] and Jenkins-Weintaub et al. [33] acknowledge the challenges associated with assessing nursing students’ clinical competencies and the inherent complexity of clinical education. The authors emphasize the importance of utilizing comprehensive assessment methods that enable thorough and holistic evaluations of students' clinical performance and their progress over time.
Study participants also expressed concerns about their need for more training in understanding and effectively utilizing the clinical evaluation method and tool. For example, a participant with a master’s degree and significant experience stated,
I don’t recall receiving any formal training on the tool... I've been using it for the past eight years, so I know how to use it, but I've noticed that some clinical instructors provide very specific comments on ways to improve or excel, while others offer more generalized feedback. For instance, they might suggest students 'seek opportunities,' but without specific examples, students may become frustrated not knowing where they can improve (Participant 8).
A study by Suplee et al. [42] is old but aligns with the findings of the current study, where a significant number of clinical instructors reported a lack of preparation for evaluating students in the clinical setting, highlighting a notable gap in their professional development. A systematic review by Wu et al. [38] supports similar findings, showing that when instructors lack training in the assessment process, their ability to fully support students is compromised. It is crucial to emphasize the role of nursing faculty responsible for clinical courses in guiding clinical instructors through the assessment and evaluation of student performance. The review also highlighted that the growing demands of teaching, research, and administrative tasks may place additional pressure on nursing faculty, potentially diverting their focus from providing this essential support. These authors and Phillips et al., [43] suggest implementing programs to address this identified gap in preparation and ensure that instructors are better equipped to fulfill their responsibilities effectively. Hence, the literature acknowledges that this deficiency in preparation could have far-reaching implications for the quality and consistency of student evaluations, potentially impacting students' learning experiences and outcomes.
Theme 3: Considerations regarding failing a student in professional practice course
Assessing students' clinical performance is a crucial aspect of the clinical instructor’s role, requiring an understanding of the curriculum and learning objectives specific to the nursing course they teach. In this study, participants talked about how they evaluate students' performance during clinical rotations and the challenges they faced. One participant, with over five years of clinical teaching experience, expressed the difficulty of this aspect of their role, stating,
Passing or failing a student is one of the most challenging parts of being a clinical instructor. It keeps me up at night...we want to support our students, but we also have to uphold university standards. It is a tough balance (Participant 6).
In this study, some participants expressed concern that certain students met only the minimum requirements to pass clinical rotations, yet their performance did not meet expected standards. These clinical instructors hesitated to fail these students, mainly if they believed the students were making progress or demonstrating minimal competency. One participant shared her experience of passing a student who did not meet course expectations. The clinical instructor advocated for a more robust and consistent evaluation process that accurately reflects students' clinical competence. The participant said,
There are no…nothing really, even though I did not, no definite thing to hinge on, what do you call passing with lower expectation, …even they are lower expectation, they barely met the course; their performance barely met the criteria…in my mind, this student should have failed in the med/surg rotation (Participant 3).
Contrary to the situation mentioned above, another participant shared her experience of failing a student and the subsequent steps taken to address the situation. The participant said, “I have failed a student, I have met with the student and the professor… I explained these are my expectations and these are their performance and depending on the progress of their performance the student failed the course” (Participant 9).
The notion of clinical evaluation has been widely discussed in nursing education literature. Gaberson and colleagues [3] emphasize the role of clinical instructors in guiding students through clinical rotations and evaluating their performance in healthcare settings. However, many clinical instructors struggle to assess students' clinical performance accurately and make decisions consistent with program standards and expectations. Dunbar [40], Glynn [44], and Pratt [21] suggest that this uncertainty arises from various factors, such as the subjective nature of clinical assessment, variations in student performance, and the absence of explicit grading criteria or guidelines. A few participants in the current study referenced this uncertainty. They acknowledged their fear that students may only meet the minimum requirements to pass clinical rotations, yet their performance falls short of the course expectations. They expressed reluctance to fail these students, which can lead to inconsistencies in evaluation practices. For instance, one participant said, “The clinical evaluation tool is set up in such a way that a student barely passes... when they are actually not passing” (Participant 12).
Some participants expressed the challenge of providing equitable mentorship to all students, especially when they must balance supporting struggling students with attending to the needs of high- performing ones. For example, one participant said, “I find it hard to help those in the middle who need assistance when I am focused on this one [student who is struggling]...I question myself, did I pass the student, if they are not... I find that difficult…” (Participant 2).
Participants acknowledge the importance of providing validation and feedback to all students but need help allocating their attention, particularly when dealing with unsatisfactory student performance. Several studies have highlighted this challenge and emphasized the significance of clinical instructors effectively managing their time during clinical rotations [40, 3, 21]. A qualitative study by Hughes et al., [45] found that evaluators' experiences and professional backgrounds are crucial in conducting clinical assessments, particularly when a student's performance is not clearly a pass or fail. These authors suggest that focusing on providing clear guidelines, along with the implementation of supportive strategies, would mitigate the challenges assessors face during clinical evaluations, especially when student performance is not easily classified as a pass or fail.
Future research in this area could focus on developing comprehensive mentorship programs for clinical instructors, aimed at equipping them with the skills to effectively cater to the individual needs of students and allocate sufficient time to each student during clinical rotations.
Theme 4: Absence of performance evaluation or feedback
Many participants emphasized the importance of receiving their performance evaluation at the end of the course. They talked about how the feedback could offer them an opportunity to modify their teaching methods and communication skills. One participant, who had been in her current role for seven years, shared, “I was called in for my evaluation, …don’t remember when … I would say, it was constructive. It helped me understand what my students want and how I can accommodate…I haven’t had any interaction with them [university] since then” (Participant 8).
Another participant said,
I always tell my students on their first clinical day…I'm here to support their learning journey, and they can talk to me about anything. Their feedback is crucial, and I see myself changing some of my practices … which help them [students] in communication with patients, in their skills or just help reduce their anxiety... I was never told by... [supervisor] about how well or... bad I am at my job... (participant laughed) ... I am happy to receive one (Participant 10).
There is considerable literature available on the importance of feedback in the clinical setting. For instance, Burgess et al. [41] suggested that effective feedback is paramount in clinical education settings, as it plays a crucial role in enhancing teaching effectiveness, promoting reflective practice, and improving student learning outcomes. Farahani and colleagues [46] emphasized implementing a structured feedback process, which improved clinical teaching effectiveness and student satisfaction with the clinical learning experience. The participants expressed willingness to receive feedback to enhance their teaching methods, communication skills, and effectiveness in facilitating student learning. With feedback, clinical instructors may feel more accountable and recognized for their efforts. For instance, a participant said, “The department [nursing school] never said anything... I am constantly looking for ways to enhance my teaching... I don’t want to continue teaching if I don’t know what kind of educator, I am…”(Participant 4).
Studies that focus on the importance of feedback suggest that it promotes accountability and transparency in clinical education. For instance, Beiranvand et al. [47] suggest that feedback encourages instructors to reflect on their practices and fosters a culture of continuous improvement to deliver high-quality education and support student success. The findings of a phenomenological study concur with the current study, where the clinical instructors value acknowledgment for their contributions to clinical education and desire a transparent evaluation process that recognizes their strengths and areas needing development [48]. While studies have examined students' perceptions of their clinical instructors' performance and teaching effectiveness [20, 49], there is a notable gap in the literature regarding the feedback clinical instructors receive from their supervisors. Given their crucial role in clinical education, further research is needed to investigate how clinical instructors receive feedback from supervisors.
Theme 5: Balancing workload and adaptation during pandemic uncertainty
The participants shared challenges they faced with an overwhelming workload during the pandemic. They discussed the transition to remote teaching modalities, which required substantial time and effort to adapt to online materials and navigate unfamiliar technology platforms.
They expressed that “the constant change and uncertainty during the pandemic were mentally draining” (Participant 12). As guidelines and protocols evolved rapidly in response to the nature of the pandemic, clinical instructors found themselves “grappling with uncertainty and ambiguity” (Participant 5). The lack of clear directions made it difficult for these instructors to plan and teach their students. A participant with a traditional teaching method said, “The transition to remote teaching was incredibly challenging...first, we did not know what we were supposed to be doing… … for me, it was constant juggling… putting more stressful hours… using the technology to teach my students” (Participant 1).
The study's findings highlight the significant workload experienced by clinical instructors during the pandemic, as supported by existing literature. For instance, Overstreet [50] found similar concerns about high-stress levels and increased workload among clinical nursing instructors teaching online during the pandemic. The author noted that stress could have resulted from inadequate preparation for the transition to online clinical education. Similarly, Keegan & Bannister [51] and Gazz [52] reported similar outcomes from the experiences of full-time nurse educators.
A few participants discussed meeting the course objectives and questioned whether their students had met the expectations. These participants were mindful of the unique circumstances of the pandemic and recognized the need for flexibility and adaptability in assessing student performance during this time. They tried to implement alternative assessment methods, provided additional support to struggling students, and explored resources to address gaps in clinical learning. A participant said,
The department was trying to redesign the curriculum and develop online materials. My group was assigned to the vaccination clinic. I was worried if my students lacked clinical exposure… whether they were meeting the objectives, and if they would pass the course (Participant 5).
Conversely, a qualitative study by Svendsen et al. [53] reported that participants were concerned about the variable quality of digital teaching methods and the impact of reduced clinical hours on student competencies during the pandemic. Similarly, Alqabbani and colleagues [54] conducted a study during the pandemic, which aligned with the current study's findings. They highlighted difficulties arising when clinical time was lost due to the transition to online platforms.
During the interview, there was a discussion about offering support to students who were grappling with personal challenges alongside their academic responsibilities during the pandemic. Some participants expressed concerns about being unable to provide adequate support and mentioned how they “struggled with the lack of face-to-face interaction with students” (Participant 3). Participants also shared how the pandemic took a toll on the mental health and well-being of their students, who experienced “increased stress, anxiety, and uncertainty” (Participant 10).
The literature on anxiety and stress among nursing students during the pandemic aligns with the findings of the current study. For instance, studies by Eweida et al. [55] and a national survey conducted by Michel and colleagues [56] reported elevated stress levels among nursing students, emphasizing the widespread impact of the pandemic on their mental well-being. Factors such as the transition to remote learning, uncertainty about clinical competencies and placements, and overall disruption to traditional educational routines likely contributed to the psychological burden experienced by nursing students and instructors. Hence, the current study contributes to the growing body of literature and emphasizes the importance of universities and institutions addressing and implementing supportive learning environments to promote the well- being of students and instructors.
Theme 6: Inadequate Instructor Orientation and Mentorship
The theme of clinical instructors expressing concerns about the lack of orientation or insufficient training underscores a critical issue in nursing education programs. Findings suggest that many clinical instructors perceive a gap in their preparedness to fulfill their roles effectively, resulting in inconsistencies in clinical instruction and potentially impacting the quality of student learning experiences. One participant recounts an incident of need for more awareness about the available resources due to inadequate orientation. The participant said, “I know they [new clinical instructors] are getting a little bit more [orientation], but I know there are many gaps.” She elaborated on an experience she encountered and said,
An instructor came to me last year near the end of the term and told me about a student struggling, and I said, 'Oh, you should be sending the student to the lab for remediation because the lab will help them…the instructor said, I did not know, and I thought, this will look poorly on me... and I feel this is a major gap (Participant 6).
Another participant raised a similar concern,
When you are starting new [CI]... I kind [of] figured things out as I went too long years into it, and I did not know… I wish I had known… I don’t think, I was provided with a skill book when I was hired first…I came in for a half-day session and met the course professor… it was overwhelming trying to figure everything out on my own, especially when it came to supporting students (Participant 7).
The current study's findings align with existing literature, emphasizing the importance of comprehensive orientation and training programs for clinical instructors. Anecdotes shared by clinical instructors in the study underscore the challenges they face due to insufficient clinical orientation, consistent with research indicating that adequate preparation is crucial for clinical instructors to support student learning effectively [57, 58]. Other studies emphasize the importance of orientations, signifying that effective programs should include information on course objectives, evaluation criteria, and teaching strategies [59, 6, 21].
A few participants also stressed the necessity of orienting both the clinical site and the unit. They highlighted the importance of instructors becoming familiar with the clinical environment, including the facility's layout, relevant policies and procedures, as well as the resources and opportunities available for students. One participant expressed, “What would be more helpful, even before you [CI] are hired, is to spend a day on the floor and have an orientation. This orientation will help instructors familiarize themselves and navigate the clinical environment effectively” (Participant 12). Another participant highlighted the need for peer coaching, stating, “The university needs to establish a system where another clinical instructor's name and contact information are provided, who can be your go-to person…similar to having a buddy. You should be able to talk to that person” (Participant 11).
It was evident from the discussion that participants were transparent and open in expressing their needs and suggesting changes the department should pursue to help them fulfill their role as clinical instructors more efficiently. The findings underscore the crucial role of training in equipping clinical instructors with the necessary skills and knowledge to facilitate and evaluate students effectively.
There is a lack of literature directly addressing orientation programs for clinical instructors in nursing [60, 61]. An unpublished Master’s thesis investigated existing orientation procedures for newly appointed clinical instructors in nursing programs across universities in Ontario, revealing a lack of uniformity in the orientation process among clinical instructors across the province. This variability leads to differences in teaching approaches province-wide. The author emphasized the need for an evidence-based standardized orientation model to promote consistent clinical education practices statewide [62]. Hutchinson et al. [60] introduced a tailored orientation program for clinical faculty from external academic institutions, which included hands-on training and mentor shadowing at the clinical site. The author reported receiving positive feedback from instructors, highlighting its quality, impact on patient outcomes, and alignment with their roles. Participants in the current study advocated for a similar program that familiarizes instructors with the clinical environment and enables them to provide appropriate guidance and support to students effectively.
Conclusion
The current study identified several critical themes related to the experiences of clinical instructors in facilitating and evaluating nursing students in professional practice courses. These findings hold significant implications for nursing education and practice. Firstly, addressing the inconsistencies and uncertainties in course expectations is crucial to ensuring that clinical instructors receive clear guidance from their course professors, enabling them to effectively facilitate their students. Providing comprehensive training and resources for clinical instructors to enhance their understanding and proficiency in clinical evaluation is essential for promoting fair and effective assessment practices. Moreover, establishing clear protocols and guidelines for failing students in clinical settings can help mitigate potential biases and ensure consistency in evaluation outcomes.
Given the challenges posed by the COVID-19 pandemic, adequate support and resources must be provided to help clinical instructors navigate the increased workload and adapt to evolving circumstances. In preparation for future public health crises or exposure events, clinical instructors may benefit from advance planning, including clear guidelines, flexible teaching strategies, and access to up-to-date training. This preparedness can help them respond more effectively while continuing to support student learning and safety. The study suggests implementing robust performance evaluation and feedback systems is vital for promoting continuous improvement and professional development among clinical instructors. Additionally, enhancing instructor orientation and mentorship programs can help address gaps in knowledge and skills among clinical instructors, ultimately improving the quality of clinical education and student learning outcomes. Future research should focus on developing and evaluating interventions to address these identified challenges and enhance the overall effectiveness of clinical education in nursing programs. Furthermore, since the pandemic has significantly affected education and clinical practice, it would be interesting to investigate how the discourse of clinical instructors facilitating nursing students has changed post-pandemic, and how these changes impact their teaching practices, student interactions, and overall clinical instruction.
Limitations
Since all participants in this study were female, it would be valuable for future studies to include male clinical instructors for comparison. This could provide a more comprehensive understanding of experiences and perspectives in clinical instruction across genders. Participants who volunteered for the study might have particularly strong or positive views about clinical teaching, which could introduce self-selection bias. One limitation of the study is the absence of atypical cases; for instance, there were no participants who had consistently positive or smooth experiences in their clinical teaching roles. This omission may have restricted the range of perspectives represented in the study.
Acknowledgements
Thank you to all the participants for their willingness to share their experiences and to the research assistants for their contributions to this study.
Conflict of Interests
There is no conflict of interest.