1. Introduction
1.1 What are the ethical implications of physical restraints for Japanese nurses?
In 2000, Japan introduced long-term care insurance, a system created in response to society’s major concern regarding the aging population and how to care for them. This system was established to assure citizens that they will receive care and be supported by society as a whole. Basically, long-term care insurance is separate from medical care insurance, and was set up as first step towards revising the structure of social security. At the same time, the Ministry of Health, Labor and Welfare passed a bill prohibiting physical restraint of older patients receiving treatment under the long-term care insurance program. As a result, it became illegal for those caring for older people in various institutions to restraint them physically. Nonetheless, in many general hospitals in Japan, physical restraint is not illegal when treating patients under medical care insurance. Nursing care continues to include the practice of physically retraining patients’, partly due to a lack of effective practices in many general wards where regulations do not specifically prohibit physical restraints. These practices are likely to continue for the foreseeable future. The continued use of restraints has been necessitated by the absence of alternative nursing care techniques to ensure the safety of older people with dementia. Patients with dementia who are hospitalized in a general hospital differ from other senior citizens who enter an institution for medical care because extra care is necessary for patients with dementia as they may remove intravenous infusion tubes and other devices; thus nurse often resort to physical restraints in order to enable treatment delivery.
Several trials have demonstrated that physical restraint, rather than protecting patients, can often cause undue harm [1-4]. Therefore, this phenomenon – whereby restraints are actively used for practical purposes but are not in compliance with current regulations - leaves nurses facing an ethical dilemma [5-8]. Several scholarly articles have addressed the challenges and conflicting feelings faced by nurses when restraining elderly patients. The placement of physical restraints by nursing staff members has been accompanied by feelings of frustration, guilt, and ambivalence [9-12].
These issues can cause nurses to question their abilities to deliver high-quality care. The stress, anxiety, and indecision they experience as a result of this ethical dilemma may also contribute poor clinical judgments.
1.2 Coping with ethical dilemmas
One of the key ethical dilemmas nurses face is the use of physical restraints, which are often necessary but are difficult to cope with [13].
Reflection and clarification of the root causes of this ethical dilemma is an important step in coping with the problem [14]. Addressing the ethical dilemma in this way can be an excellent opportunity not only to improve nurses’ job satisfaction but also to improve the quality of care delivered. To develop programs aimed at achieving this, it is first necessary to understand the coping strategies nurses currently use to cope with ethical dilemmas [15-17]. Moreover, this study sought to clarify the relationship between a nurse’s exposure to elderly relatives and their perspective in using restraints on the elderly in health care situations.
1.3 Study Objectives
The present study aimed to clarify factors surrounding the dilemma of using physical restraints on elderly patients with dementia. In particular, we surveyed how nurses who live with elderly relatives coped with this issue.
2. Methods
Subjects and Data collection: Perspectives on this dilemma differ by individual, and are affected by educational background, experiences both in nursing and in one’s own life, and by each individual’s value system [10-12]. Subjects were selected using the purposive selection method [18] at community hospitals in mid-western Japan. Selection criteria for hospitals required that they 1) contained an independent nursing division or department in the hospital under nursing management, 2) offered a postgraduate study or educational program for nurses, 3) provided similar employment conditions for all nurses who served as subjects for our study, and 4) served as a general hospital. Study objectives and methods were explained to individuals in charge of nursing at the 3 selected hospitals. We enrolled 269 nurses who worked in general wards of the 3 hospitals and who agreed to participate in the present study.
Ethical considerations: The study was performed using an independently prepared questionnaire. Study participants were informed of the study objectives, methods of questionnaire distribution and recovery, and addresses of the investigators in one of the following ways: 1) we distributed request sheets disclosing this information, or 2) investigators explained this information to the individuals in charge of nursing at the hospital/ward at the time of the interview. Request sheets sent to individuals disclosed the definition of “physical restraint” and “elderly patients,” instructions on completing the questionnaire and the period of response, and the present study objectives. Investigator addresses were enclosed to help nurses better understand the study. The questionnaire was designed to ensure subject privacy. Specifically, interviewees were allowed to complete the form themselves and remain anonymous. The questionnaire was constructed so that, when completed, it could be inserted in an envelope distributed in advance to the subjects who could seal it themselves. Subjects were asked to return the completed questionnaire in the sealed envelope to a designated place, roughly two weeks after distribution. Head nurses for the wards were asked to collect completed questionnaires in the sealed envelopes and return all of them together to those in charge of the study. This study was approved by the Ethics Committee of the Nursing Department of the Meiji University of Integrative Medicine.
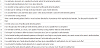
Extraction of dilemma coping items: We developed a 16-item survey to assess dilemma coping items (Table 1). Coping with ethical dilemmas can be divided into the following three content areas: (i) positive cognition and actions (Items 1-9); (ii) negative cognition and actions (Items 12-16); and (iii) choosing not to act, or maintaining the status quo (Items 10-11). Each of the survey questions was based on a four-point Likert scale, with higher scores indicating good coping strategies. When faced with the dilemma of physically restraining an older person with dementia, we assumed that nurses used one of the three coping methods. “Positive cognition and actions” would involve a nurse solving a dilemma in a positive manner, with the intent to resolve the problem (e.g., some nurses held conferences to consult with experienced senior nurses about the issue of restraining patients). “Negative cognition and actions” would involve nurses avoiding the dilemma (e.g., some nurses either refused to work with patients with dementia, or reminded themselves that the patient would leave soon and therefore did not give careful thought to the situation). “Choosing not to act, or maintaining the status quo” involved nurses accepting the present situation and doing nothing to resolve the problem (e.g., some nurses who felt inexperienced with regard to dementia care thought it to best to follow the doctor’s instructions without questioning the situation). A preliminary test was conducted among 10 nurses working in orthopedic surgery wards at community hospitals, and the results from this test were used to improve the questionnaire. Data obtained from the modified questionnaire were analyzed in the present study.
Validity and reliability of dilemma factors: Reliability of the constructed items within the dilemma was examined using a Cronbach’s α coefficient of 0.6 or greater to test for internal consistency. Factor structure was confirmed following factor analysis (maximum likelihood method: promax rotation) for construct validity. Criteria for sample validity for the factor analysis targeted a Kaiser-Meyer- Olkin (KMO) value of 0.6 or greater and a cumulative contribution ratio of 60% or more. Item exclusion was applied to a factor loading of 0.4 or greater without difficulty in interpretation.
3. Results
3.1 Adequacy of item selection and dilemma coping factors
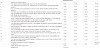
The 16 dilemma coping items were subjected to a factor analysis (maximum likelihood method: promax rotation) to clarify dilemma coping factors among nurses who live with elderly relatives. Items with either a factor loading of 0.4 or less or difficulty in interpretation were deleted, and the final remaining 14 items were used for analysis. We extracted four items with a characteristic value of one or greater, which yielded a significant KMO value of 0.79 and a cumulative contribution ratio of 66.8%. Cronbach’s α coefficient for composing items of each factor were 0.87, 0.83, 0.60, and 0.68 for factors 1, 2, 3, and 4, respectively (Table 2).
3.2 Ethical considerations
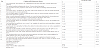
The same procedure as described above was performed for the 16 dilemma coping items among nurses who did not live with elderly relatives, which resulted in a total of 16 final items used in the analysis. Three items with a characteristic value of one or greater were extracted, revealing a significant KMO value of 0.78 and a cumulative contribution ratio of 56.8%. Cronbach’s α coefficient for composing items of each factor were 0.84, 0.85 and 0.79 for factors 1, 2, and 3, respectively (Table 3).
4. Discussions
We extracted deferent factors with regard to the dilemma faced by nurses concerning the physical restraint of elderly patients. We found that exposure or living with elderly relatives influenced nurses’ coping with this dilemma. Finally, we dedicated a limitation of this study; the use of a questionnaire is a limitation of this study.
However, the current data are promising, although further studies and a better standardization of methods are needed to obtain clearer results. Future studies should consider the possibility of approach to model for support coping with the dilemma of using physical restraints on elderly people with dementia by perspectives from nurses who live with elderly relatives.
Competing Interests
The authors declare that they have no competing interests.
Author Contributions
All the authors substantially contributed to the study conception and design as well as the acquisition and interpretation of the data and drafting the manuscript.