1. Introduction
Pilonodal disease is a common problem in young people, affecting most commonly men between the 2nd and 4th decade of life [1]. Patients may present with symptoms of acute disease (pain in the sacrococcygeal region due to abscess formation) or may suffer from the chronic form of the disease with purulent discharge from one or multiple sinus tracts [2]. However, there is still no consensus as for the ideal treatment of this disease [3]. Often, the method applied relies solely on the preference of the surgeon and his familiarity with each technique [4]. During the recent decades, in the context of less invasive surgical procedures being more broadly used in everyday clinical practice, several non-surgical or less aggressive surgical techniques have also been tested in the treatment of pilonidal cyst. The present study aims at presenting our initial experience in the outpatient treatment of pilonidal disease using a 1470 nm diode laser.
2. Material and Methods
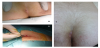
Five patients (3 male, 2 female) were treated with a diode laser at wavelength of 1470 nm by means of a radial fiber (Biolitec Biomedical Technology GmbH, Jena, Germany) in a day-case private center (Iasi Private Medical Center, Ioannina, Greece) on an outpatient basis. All had an unremarkable personal medical history except for a male patient suffering from Crohn’s disease. Ages were 15, 17, 20, 21 and 26 years (Table 1). One patient had been treated surgically with the lay-open technique under general anaesthesia twice before the laser procedure (at 11 and 6 months prior to laser application), suffering from a large disfiguring scar with 3 purulent sinuses (Figure 1). Two patients had had an acute abscess during the time of their first visit in our center and were thus treated with drainage through a small incision (without antibiotics) to allow for faster recovery before applying the laser energy. Patients with primary chronic disease presented with complaints of intermittent itching or discomfort in the sacrococcygeal area and small serous discharge from the existing sinuses. These symptoms were initiated between 4 and 11 months prior to patients’ admission.
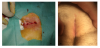
Patients were treated in the supine position under local anaesthesia using a combination of 10 ml lidocaine 2% and 10 ml ropivacaine 7,5% for infiltration of the skin and subcutaneous fat surrounding the sinuses, after cleansing of the skin with povidone iodine solution. All external sinus openings were widened using a thin Kelly clamp and in two cases were the sinuses showed signs of granulation they were superficially excised in a similar manner with that used in the pit-picking technique. All sinuses were explored using a thin metallic probe, then cleansed off of hair and debris and irrigated with hydrogen peroxide and normal saline. Then the optical fiber (radial emission energy at 1470 nm wavelength) was inserted in each sinus separately and the energy applied was 10 Watt pulsed (1 Sec ON – 0,5 sec OFF), aiming at an average portion of energy around 100-110 J/ cm. Successful application of the energy was witnessed immediately as primary closure of the fistula tract, with inability to re-enter the optical fiber at the sinus already treated. After applying energy to all sinuses and their bifurcations, the wound was covered with ointment and sterile gauze.
Total time of the procedure included administration of local anaesthesia, clearing of the sinuses, laser application and wound packing. All patients were discharged 1 hour after the procedure with painkiller administration (1 g of paracetamol per os) on demand. During the first week the patients were advised to apply a nonpharmaceutical local ointment and one sterile gauze on the area once daily. At the end of the first week patients were examined by the surgeon and were then advised to take proper baths and cover the area with simple gauze for the rest of the healing time. Visits to the surgeon were
3. Results
All patients were treated successfully under local anaesthesia with application of laser energy at 1470 nm during a single visit. Portion of energy applied varied between a total of 417 and 1197 J (mean 118 J/ cm of sinus treated). Mean time for the completion of the procedure was 43 min (range 18-58). All patients advised to receive common painkillers (paracetamol and/or COX-2 inhibitors) per os in case of experiencing pain, but no one reported any painkiller use after discharge. No antibiotics were prescribed for prophylaxis against local infection. Application of local ointment and gauze over the wound was reported to be well tolerated from the patients. Return to normal daily activities (4 out of 5 were students) was possible for all patients after two days. Healing times varied between 3 and 6 weeks (mean 5 weeks) and were well tolerated by the patients, except for two that complained for mild irritation of the skin due to gauze application. Follow-up at 3 and 6 months confirmed complete epithilialization of the sinus tracts and resolution of symptoms. No disfiguring scars were developed and the aesthetic results were highly praised by all patients (Figures 1 and 2).
4. Discussion
Pilonidal disease affects mostly men of a young age [4]. The aetiology of this disease is still unclear, once thought to be a congenital but nowadays it is clear that it is an acquired one [1,3]. Some predisposing factors have well been recognized, such as obesity, a deep natal cleft, excessive hair covering the sacrococcygeal region, wrong sitting position or minor trauma of the region and [3,5].
This gap in our understanding of the disease is mirrored in the multiple techniques that have been developed over the years. Surgical excision of the cyst together with the accompanying sinuses seems to be the method with the greatest appraisal [4]. The wound may be left to heal by secondary intention leading to prolonged healing times and severe patient discomfort (pain during open wound cleaning, serous discharge, absence from work etc) or it may be primarily suture-closed, thus subjecting the patient to potential wound infection or even wound break-down [1,6]. More aggressive surgical methods such as Karydakis operation and the Limberg-flap technique have been developed in an effort to completely eradicate the disease and minimize the risk of recurrence [5,7]. However, all the above mentioned ‘highly invasive methods’ usually require general anaesthesia, prolonged hospital stay (at least 2-3 days), debilitate the patient during the first post-operative days and cause significant postoperative pain requiring painkiller use [2,8].
Less aggressive techniques have also been employed, such as sinotomy [9], the pit-picking technique [10], obliteration of the cyst through phenol injection with or without depilation with multiple results [3,11,12]. Laser treatment has emerged as a minimal invasive procedure starting from the treatment of anal fistula [13,14]. The present paper reports our initial experience with treating primary and recurrent pilonidal sinus disease. This is a small case series of five patients with different number of sinuses treated, both primary and recurrent. All patients were treated on an external basis, under local anaesthesia, without the need for painkiller use at home. After a short follow-up time not exceeding six months there were no recurrences documented and patients were enthusiastic in being treated with such a simple and painless method.
Literature reports regarding the use of certain types of laser (CO2, Nd: YAG, xenon etc) are scarce [15-19]. All report satisfactory results with a single or multiple applications, performance of the procedure in an office setting with minor patient discomfort and good results in terms of recurrence and cosmetic result. The present study has some limitations; the small number of patients involved, the short followup period and the treatment of a unanimous patient group (in terms of number of sinuses treated, treating both primary and recurrent sinuses, co morbidities etc). However, initial experience is more than encouraging and shows promising results with this new method, which is simple, safe and offers definite treatment without the need for more extensive surgical procedures, while the final cosmetic result is excellent. Healing times may be somewhat long, but there is no patient discomfort or activity restriction, absence from work is minimal and the procedure can be repeated in case of recurrence.
5. Conclusion
In conclusion, obliteration of the pilonidal cyst together with the accompanying sinuses with laser energy application seems to be a good alternative to more extensive surgical procedures.
Competing Interests
The authors declare that they have no competing interests.