1. Background
Schizophrenia is a very disabling disease with a significant proportion of patients having more than one episode of acute psychotic symptoms [2]. The main reason for a relapse is nonadherence, followed by age of onset, justifying the use of long acting injectable antipsychotics (LAI) [3].
Atypical antipsychotics have been associated with a lower risk of extrapyramidal symptoms but a higher risk of metabolic adverse effects. They became the first line therapy in the last few years and it is suggested that atypical LAI could outperform oral medication [4]. Despite the prescription of LAI, patients still relapse, having new psychotic episodes. In the last few years there is growing evidence regarding the recognition of subsyndromal symptoms, as they may be important to prevent further escalation of psychotic symptoms and re-admissions.
According to previous studies, anxiety was found in 41.5% of patients with schizophrenia. Patients with anxiety symptoms evidence higher functional impairment, mainly in the professional and social functioning. The group of patients with comorbid anxiety disorders showed higher positive symptoms and were more often under treatment with antianxiety drugs. Contrasting, they had lower number of hospitalizations [5]. Huppert et al. also showed that quality of life was also affected by the presence of anxiety and depression. Particularly, anxiety was associated with bigger difficulties in daily life activities such as family and social activities, despite the control of positive symptoms [6].
Antidepressant and anxiolytic medication are frequently used as co-adjuvant therapy in schizophrenia. The CATIE trial showed that at baseline 38% of patients were prescribed antidepressants and 22% anxiolytics. There was an association with the presence of anxiety or depression, being female, and being treated with second-generation antipsychotics. Depressive mood showed only partial response with this approach [7].
At follow-up in the same trial, a higher positive symptom score and younger age were associated in an earlier prescription of antidepressants. The duration of antidepressant treatment was longer in patients with lower education and in those with a history of alcohol use disorder. Predictors of anxiolytic initiation were being separated/ divorced, not being African-American, younger age, higher body mass index and akathisia [8].
Ritsner et al. showed that patients with schizophrenia treated with antidepressants and anxiolytics have better quality of life [9].
Regardless of these findings, some evidence shows a 4.8-fold higher mortality risk with the chronic use of anxiolytics (including cardiovascular and suicide-related mortality). This could be associated with the illness severity or comorbid anxiety. An increased risk for accidents due to daytime sedation or cognitive impairment is another hypothesis [10]. Particularly, the deleterious cognitive effect was suggested to be associated with impaired attention/working memory, independently of socio-demographic variables and illness characteristics [11].
Our aim is to study the possible association between hospital admissions and emergency department visits among schizophrenic patients who had been prescribed anxiolytic medication. We compared two groups, considering oral vs long-acting injectables and concomitant medication.
2. Methods
We conducted a post-hoc analysis of a three-year prospective cohort study in a community mental health team (CMHT) in Portugal, urban area. We included all patients with the diagnosis of schizophrenia according to the International Classification of Disorders, version 10th, published by the World Health Organization, aged 18 years and above and followed during 2015 in the CMHT. The study was approved by the ethical committee of our hospital.
Several demographic and clinical baseline characteristics were recorded, and the primary outcome was psychiatric admission. We included emergency department visits (ED) and occupational status as secondary outcomes.
Parametric tests (χ2 test, student t test) were used for statistical analysis according to the variable type. Statistical significance was set at 0.05.
We categorized the antipsychotics available in Portugal according to the Neuroscience based Nomenclature (NbN)1: Receptor antagonist (RA) (D2) amisulpride, haloperidol, fluphenazine, pimozide, sulpiride, e zuclopenthixol; RA (D2, 5-HT2) cyamemazine, chlorpromazine; levomepromazine , flupentixol, melperone, olanzapine, ziprasidone, zotepine; RA (D2, 5-HT2, NE alpha-2) clozapine, paliperidone e risperidone; Receptor partial agonist (RpA) (D2, 5-HT1A) and RA (5-HT2A) aripiprazole; RA (D2, 5-HT2) and reuptake inhibitor (NET) quetiapine.
3. Results
According to our selection criteria, 145 patients were selected. In the early follow-up period, we had 15 dropouts mainly because of change of address. In the remaining group (130 patients), 62.8% were males, with a mean age of 47 years (standard-deviation [SD] of 12.9 years), mainly unemployed (37.7%) or retired due to disability (20.7%), with a mean duration of illness of 8.7 years (SD 3.1 years).
At baseline, 48.5% were prescribed with one oral antipsychotic (OA). In the group of patients taking LAI, 94% were additionally prescribed with OA. In the group of patients taking only OA, we found that 41% were prescribed with more than one antipsychotic. Mood stabilizers were prescribed in 21.5% patients, antidepressants in 40%, anxiolytics in 50% and hypnotics in 13.1%.
Table 1 presents the social-demographic and main differences between the two groups: OA and LAI. We found a higher prescription of antipsychotic polypharmacy in the LAI group, which was statistically significant (p-value <0.001), mainly regarding the receptor antagonist D2 class (p-value <0.001), receptor antagonist (D2, 5-HT2) and reuptake inhibitor (NET) class (p-value 0.020).
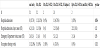
In Table 2 we present the differences between oral medication and LAI classes according to NbN. We found that the difference between groups regarding antipsychotic polypharmacy in the LAI group was statically significant (p-value <0.001), with almost all the patients taking LAI being prescribed with RA (D2) (p-value <0.001), RA (D2, 5-HT2, NE alpha-2) (p-value 0.008) and RpA (D2, 5-HT1A) and RA (5-HT2A) (p-value 0.004) classes.
The individual analyses showed that in the LAI group the use of antipsychotics is not restricted to their own class. The RA (D2) class (52 patients) had 69% use of OA of the same class, but also 42% of RA (D2, 5-HT2), 46% of the RA (D2, 5-HT2, NE alpha-2) class, 8% of the RpA (D2, 5-HT1A) and RA (5-HT2A) class and 31% of the RA (D2, 5-HT2) and reuptake inhibitor (NET) class. The RA (D2, 5-HT2) class (2 patients) had 50% prescribed of the RA (D2), RA (D2, 5-HT2) and RA (D2, 5-HT2) and reuptake inhibitor (NET) classes. The RA (D2, 5-HT2, NE alpha-2) class (23 patients) had prescribed 83% of the same class, and 13% of the RA (D2) class, 35% of the RA (D2, 5-HT2) class, 13% of the RpA (D2, 5-HT1A) and RA (5-HT2A) class and 22% of the RA (D2, 5-HT2) and reuptake inhibitor (NET) class. The RpA (D2, 5-HT1A) and RA (5-HT2A) class (2 patients), had 100% prescriptions from the RA (D2, 5-HT2, NE alpha-2) and RpA (D2, 5-HT1A) and RA (5-HT2A) classes and 50% in RA (D2, 5-HT2) and reuptake inhibitor (NET) class.
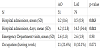
Our primary outcome was hospital admissions. Patients in the OA group had fewer admissions (p-value 0.043) and a shorter hospitalization (p-value 0.041) (Table 3). The Receptor antagonist (D2) LAI class was the closest to oral antipsychotics group (Table 4). Comparing the LAI RA (D2) with OA, there was no statistical significant difference (p-value 0.343). Comparing the LAI RA (D2, 5-HT2, NE alpha-2) with both OA and LAI RA (D2), there was a significant difference, disfavoring the LAI RA (D2, 5-HT2, NE alpha-2) class (p-value 0.003 and p-value 0.032, respectively).
We analyzed known associations between baseline variables (age, sex, education, occupation, illness duration and medication) and hospital admissions. Only duration of illness (p-value <0.001) and being prescribed with anxiolytics (odds-ratio 2.8; p-value 0.015) at baseline were associated with hospital admissions. Higher duration of illness showed a protective effect and anxiolytic prescription a negative association. Patients taking more than one antipsychotic were not associated with a higher number of admissions (p-value 0.778).
The secondary outcome was emergency department visits. We did not found any association with the prescription profile. Having a work occupation showed only a statistical trend (p-value 0.071), higher in the OA group.
4. Discussion
We present a real-world analysis of patients diagnosed with schizophrenia followed in a CMHT in an urban area of Portugal.
Some authors argue that LAI can be used without any other antipsychotic, justifying their use to improve adherence [4]. In our study we found an association between antipsychotic polypharmacy and LAI prescription. This finding could suggest that more resistant disorders are treated with antipsychotic polypharmacy. According to this hypothesis, a higher number of hospital admissions was expected, but in our results, there was no difference in hospital admissions. We could argue that the polypharmacy came from the same class, but in the two major LAI classes, more than 50% of patients were taking oral medication with a different profile from the LAI classes.
According to these findings, we acknowledge that the monotherapy with a LAI antipsychotic may not be possible for a considerable number of patients, which contrast with internationally recognized clinical guidelines. In clinical practice, we discuss with patients that LAI could be a way to avoid oral medication but, according to our results, this argument should not be used to promote the introduction of LAI.
Regarding our primary outcome, hospital admissions, we found that patients in the OA group had fewer number and duration of admissions. The Receptor antagonist (D2) LAI class with the oldest LAI, is the only one to approach the OA values. A discussion about the efficacy of the newest LAI (at least risperidone and paliperidone, because the sample is too small to compare with aripiprazole) could be carried out, but we didn’t have the sample size to allow it.
As expected, longer duration of illness showed a protective association against new admissions.
We also found a higher use of anxiolytic medication in the subgroup of risperidone and paliperidone. Is this an effect of these particular antipsychotics or a characteristic of the particular patients? We could argue that this association may be related to the side effects profile of these two related antipsychotics. Unfortunately, we did not include a screening tool regarding side effects in our study, and this question remains to be answered.
The prescription of anxiolytics at baseline showed a negative association with hospital admissions. Previous research showed ambivalent results with this therapeutic approach, probably because anxiolytic medication hides more profound problems, such as resistant positive symptoms, comorbid anxiety disorder, lack of employment, unstable and negative family and social relations, or the consequences of antipsychotic polypharmacy [8,10]. This group of patients should be further studied to understand the underpinnings of this association.
Our results evidence the need to implement non-pharmacological interventions focusing anxiety on patients with schizophrenia.
Our study has several limitations. The overall sample size is small and in some LAI classes impeditive of statistical analyses. In the inclusion criteria we considered patients with previous diagnosis of schizophrenia, and we did not assess the severity of positive and negative symptoms with standardized scales during the study. The absence of screening for side effects between groups is also a limitation. The study has the limitations regarding the chosen design. Larger and multicentric prospective cohorts are needed to clarify the results.
5. Conclusions
Our findings support that OA are more effective in preventing hospital admissions and duration of admission than LAI. The emergency department visits and occupation status showed no statistical association, but only a trend favoring OA regarding work. Being prescribed with anxiolytic medication is associated with a worst outcome regarding hospital admissions and this group of schizophrenic patients should be further investigated. Larger and multicentric prospective cohorts are needed to clarify the effects of particular classes of antipsychotics in the long-term prevention of admissions, symptomatology and remission. Anxiety and anxiolytics should be further investigated in schizophrenia.
Competing Interests
The authors declare that they have no competing interests.
Author Contributions
Carla Spínola made contributions regarding conception and design,
data collection and writing and revision of the manuscript.
Daniel Neto made contributions regarding conception and design,
data analyses, writing and revision the manuscript.
Leonor Santana made contributions regarding conception and design,
data collection and writing and revision of the manuscript.
Joaquim Gago made contributions regarding conception and design,
writing and revision of the manuscript.
All authors gave final approval of the version to be published.