1. Introduction
Although seat-belt induced aortic injuries occurring in restrained occupants involved in motor vehicle collisions were well recognized and reported in literature, the term “Seat-belt aorta” was first introduced by Dajee, et al in 1979 [1]. Seat belt aorta is a potentially fatal, rare injury that typically involves acute aortic intimal tear with, variably, consequent dissection caused by direct compression of the aorta against the vertebrae [2-3]. Other patterns of injury include partial or complete aortic occlusion, disruption of the aortic intima and media with the subsequent pseudoaneurysm development and aortic rupture with active hemorrhage [3].
In addition, blunt abdominal trauma associated with the use of seat belts in motor vehicle collisions may not only result in aortic injury but it may also be associated with intra-abdominal and spinal injuries and this leads to what is known as “seat-belt syndrome”. Seat belt syndrome was first described by Garrett and Braunstein in 1962 [4-5]. Thereafter, it has been extensively described in literature with numerous case reports of abdominal wall disruption, hollow viscus, solid visceral and spinal injuries related to the use of seat-belts.
We report a case of seat-belt syndrome with abdominal aortic intimal tear and dissection which was successfully managed with endovascular treatment.
2. Case Report
A 25 years old man, a restraint co-driver by a 3-point seatbelt, was brought to the Emergency Department at Al Ain Hospital after being involved in high speed motor vehicle collusion. He was conscious and complaining of neck and abdominal pain with shortness of breath. His heart rate was elevated (HR 126 b/m) but otherwise homodynamically stable. Physical examination revealed a wide band of contusion and ecchymosis extending obliquely over the chest and transversely over the lower abdomen, the ‘seat belt sign’. The right side of the neck and left side of the chest were tender. The abdomen was distended, tender with evidence of peritoneal irritation. The femoral pulses were equally palpable.
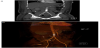
An urgent contrast-enhanced CT scan of the neck, chest, abdomen and pelvis demonstrated rectus abdominis muscle rupture with herniation of the bowl loops. There was evidence of distal abdominal aortic contusion just above the bifurcation with linear intraluminal filling defects extending to left common iliac artery, which could be due to intimal flaps or clots (Figure 1a and 1b). A large periaortic/ retroperitoneal haematoma was seen compressing the IVC. No hollow viscus or solid organ injury was demonstrated. There were fractures of the right C5 transverse process, proximal sternum fracture and multiple left-sided ribs.
Immediate exploration laparotomy demonstrated more than 15 cm mesenteric tear involving the ileocecal junction with devitalization of the terminal ileum which was managed by terminal iliem resection and limited right hemicolectomy with side to side ileocolic anastomosis. Exploration of the retroperitoneum revealed aortic intimal tear involving 5 cm of the infra-renal aorta with no active bleeding and retroperitoneal haematoma. No intervention was made for the aortic injury since there was no active bleeding and intension for endovascular treatment was made. No other visceral injuries were identified and the rectus muscle was repaired.
The following day, the patient was brought to the angiography suite and diagnostic angiography of the abdominal aorta showed a segmental (~9 3 cm long) stenosis of about 70% of in the lower abdominal aorta due to intimal tear with consequent dissection from the traumatic blunt aortic injury with extension into the common iliac arteries (Figure 2). Angioplasty of the stenotic segment was performed with two covered stents (ATRIUM VL12 12mm x 29mm). Completion angiogram demonstrated good stent placement with resolution of the dissection of iliac arteries and no immediate complications (Figure 3).
The patient tolerated the procedure well and he was doing fine. One week follow up abdominal contrast-enhanced CT scan illustrated good placement of the aortic stent within the infra-renal aorta with reduction of the retroperitoneal haematoma and no evidence of leak (Figure 4a and 4b).
The postoperative hospital course was complicated with intraluminal bleeding at the bowel anastomosis noted on 16th postoperative day (Figure 5). A trial of bleeding control with colonoscopy failed. Successful endovascular embolization of the bleeding vessel from superior mesenteric artery was accomplished using 2 metallic coils (Figure 6a and 6b). Following discharge, subsequent follow up was uneventful.
3. Discussion
Despite the fact that passive restraints have significantly reduced mortality and critical injuries from motor vehicle collisions [6], it has, in the contrary, been incriminated in causing serious blunt abdominal aortic traumas [7-8]. Fortunately, such injuries are rare but the true incidence is unknown [3]. Freni, et al estimated the incidence of blunt abdominal aortic injury to range between 0.01% and 0.07% [3].
Most of the blunt aortic injuries occur in the thoracic district, whereas blunt abdominal aortic injuries are far less common and probably accounting for less than 5% [3].This is believed to be explained by the relatively secured retroperitoneal location of the abdominal aorta [7].In most of the cases where the abdominal aorta is injured, the infra-renal portion is the typical location of injury [7].
Seat-belt syndrome is commonly linked to the two-point restraints (lap-belts) [5-9]. It is suggested by George, et al that the type of restraints contributes to the pattern of injury [5]. Conversely, Catherine, et al found a similar pattern of injury exhibited by both the two-points and three-point restraints [10]. Additionally, improper positioning of the restraint was identified by Sato to be the cause of serious and fatal injuries in belted occupants [11]. Likewise, Lutz, et al reported that hollow viscus injuries may be directly related to improper restraint with a 4-fold increase in risk when compared with solid visceral injuries [12].
To appreciate the mechanism of injury, it is essential to recognize that the seatbelt redistributes and transfers the kinetic energy attained in a motor vehicle collision to the less susceptible pelvic region [5]. This rapid deceleration may result in direct compression of the intra-abdominal viscera and the abdominal aorta against the spine [7]. Instead, the abdominal aorta may be subjected to indirect forces acting upon its high-pressure blood column leading to stretching and shearing of its wall [7].
A high index of suspicion is critical in identifying patients with seat-belt syndrome as occasionally the initial clinical picture may be ambiguous with no definitive indication of early intervention. Berthetet al, stated that the rate of delayed diagnosis may reach up to 34.3% [13]. Acute arterial insufficiency was described by Roth, et al. to be the most common early sign [14]. Yet, in the presence of intra-abdominal visceral injury, acute abdomen is the most common clinical presentation [3]. The classical seat-belt sign, i.e., bruising and ecchymosis caused by the seat-belt, may point out to an internal injury in about one third of cases as indicated by Hayes et al [15-16].
It is worth mentioning that the clinical pattern of presentation varies according to the spectrum of injuries incorporated in seatbelt syndrome. These include abdominal wall ecchymosis, intraabdominal, aortic and lumbar spine injuries. The intra-abdominal injuries include mesenteric tears, hollow viscus perforation and injuries to solid organs. Different patterns of aortic injuries yield variable clinical manifestations which may include retroperitoneal hematoma, bowel and peripheral ischemia; anterior spinal artery syndrome and hypovolemic shock [3-7].
Chance fracture (also known as the seat-belt fracture), i.e., transverse fracture of the lumber vertebra with horizontal splitting through the spinous process, is the classical spinal injury seen in seatbelt syndrome [5-17]. It is believed to result from the extreme flexiondistraction of the spine around the seat-belt and it is most commonly found in the upper lumber vertebrae [5,7-18].
Variety of thoracic injuries was associated with the use of three-point restraints in motor vehicle collusions [15]. These vary from simple skin abrasions and thoracic cage fractures to disastrous thoracic aortic transection, massive lung laceration, cardiac and carotid injuries. Seatbelt sign seen at the neck and chest should prompt a conscientious workup to exclude the coexistence of these injuries. Nevertheless, the three-point restraints were found to be more protective for lumbar fractures as described by Catherine et al [10].
At all times, management should be tailored to the individual case presentation. In hemodynamically unstable patients, immediate exploration may be life-saving. On the other hand, most stable patients with blunt abdominal aortic injury are potential candidates for endovascular treatment [19]. The utility of CT scans, angiography and ultrasonography aids comprehensive assessment and management planning in these patients [20].
Endovascular treatment has proven to be a successful advancement in the management of vascular trauma. Numerous case reports established the efficiency of endovascular management in blunt aortic injury since the first report of successful endovascular repair of a traumatic abdominal aortic dissection by Marty-Ane et al. in 1996[20-26].
The prognosis is principally determined by early recognition of aortic injury and prompt management. In review of the literature, it is devastating to realize that the mortality rate may reach up to 37% [21]. It is also essential to recognize the delayed diagnosis is a major predictive factor for morbidity even after treatment [3]. Freni, et al indicated that aortic occlusion may lead to lower limb and spinal ischemia which may eventually progress to irreversible paraplegia or even major amputation if not recognized and acted upon early [3].
4. Conclusion
Seat belt syndrome remains a potentially fatal injury with the mortality rate reaching up to 37%. A high index of suspicion is critical for early detection of the possible injuries involved in the spectrum of seatbelt syndrome. Occasionally, the initial clinical picture is ambiguous and the patients may be asymptomatic. The existence of convincing clinical evidence of blunt aortic injury should prompt extensive workup and immediate management.
Endovascular treatment, a major advancement in the management of vascular trauma, has revealed successful outcomes in several case series available in the literature. We believe that almost all hemodynamically stable patients need be accessible to endovascular treatment in the appropriate sitting.
Competing Interests
The authors declare that they have no competing interests.
Author Contributions
The author substantially contributed to the literature review, drafting the manuscript and approve the final version of the manuscript.