1. Introduction
Ischemic heart disease is a multifactorial entity that can be diagnosed through non-invasive tests such as nuclear cardiology examination and computed tomography (CT) [1]. The stress myocardial perfusion imaging plays an important role in the risk-stratification of the patients with suspected coronary artery disease, diagnosing the extent and severity of infarction and ischemia induced by both epicardial coronary arteries and resistance vessels [2]. CT coronary angiography can help identify morphological features of coronary arteries [3-4]. If the ischemia-causing coronary stenosis is identified by non-invasive imaging,the culprit lesion can be determined as a therapeutic target of coronary intervention [5]. The relationship between ischemia and coronary artery narrowing can be accurately diagnosed by fusion imaging between single photon emission computed tomography (SPECT)and CT coronary angiography [5]. On the other hand, if the patients with coronary stenosis had developed rich collateral coronary circulation, no ischemic findings on myocardial perfusion imaging might be observed [6]. Additional information on vessel calcification and inflammation can be identified by the CT and the 18f-fluorodeoxyglucose-positron emission tomography (FDG-PET) in the process of coronary artery disease, as well as ischemia and infarction [7]. Recently non-invasive imaging has advanced recently in the field of the nuclear cardiology, includingof SPECT / CT with multifocal collimator and semiconductor detectors, enabling a short acquisition time [8-9]. The SPECT/CT also becomes available and quantifies calcification and cardiac function. This article describes a method of diagnosing though hybrid information from multiple modalities in characterizing the pathophysiology of coronary artery disease.
2. Anatomic and Physiological Stenosis
Anatomical information of the coronary arteries can be easily obtained by CT angiography [3-4]. Coronary stenosis is critical target in a strategy of coronary intervention therapy [5]. However, not all of these pathophysiological conditions can be diagnosed by CT information, since small arteries and arterioles level as well as the epicardial coronary artery plays an important role in controlling the coronary circulation at the same time [10]. Actually coronary stenosis on CT may not induce ischemiaon SPECT images [11-12]. Reduced coronary flow reserve might be observed in patients without stenosis [10,13]. Myocardial perfusion tracers as 201Tl or 99mTc agents will be distributed according to the antegrade blood flow and the amount of coronary flow, and also depends on the blood flow of the collateral circulation. Understanding of these physiologiesis essential in order to interpret well a hybrid or fusion imaging.
In addition to the detection of coronary stenosis, important information such as coronary plaque, vascular remodeling, microcalcifications and the myocardial wall thickness could be obtained by the CT scan. Coronary plaque morphology had been intensively investigated [14-15]. There was a good agreement between CT angiography plaque and intravascular ultrasound [16]. Low density CT density or napkinring sign plaque, and thin capfibroatheroma are considered to be suggestive feature for the unstable condition [17-18]. However there might be a long way to use CT plaque information as a clinical indicator for evaluating the prognosis of the patients with stable angina pectoris.
3. Quantitative Evaluation of Myocardial Ischemia
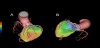
The Courage trial nuclear sub-study showed that the subjects with improved perfusion had better prognosis than those without, by using myocardial perfusion imaging [19]. And, the beneficial prognostic result was observed in the patients especially with more than 5% ischemic improvement through coronary intervention. The incidence of cardiac events for the patients with coronary artery disease becomes higher according to the degree of perfusion defect in stress myocardial perfusion scan [2]. The prognosis of the subjects with coronary artery disease is reportedly improved by performing coronary intervention in patients with more than 10% ischemia. Therefore, the quantification of the degree of ischemia or infarction is so important in selecting subjects to treat for improving the prognosis. Without using invasive methods such as fractional flow reserve (FFR) measurement by cardiac catheterization, a recent study demonstrated that myocardial perfusion imaging could identify the lesion to be accurately evaluated by non-invasive stress SPECT [21]. Recent advancements of nuclear cardiology techniques support this analysis by novel software. The neural network software called cardioREPO (Fuji Film RI Pharma, Tokyo, Japan), which was developed in collaboration with Exini Co., Sweden.This software can identify the blood flow abnormalities and myocardial ischemia in quantified analysis [21]. Since the amount of ischemia is closely related to the subsequent cardiac death, the precise analysis of myocardial ischemic area would becomeso important (Figure 1). Only patients with decreased ischemia demonstrated in myocardial imaging have the benefits of revascularization, including bypass surgery [19]. Meanwhile, when the subject with suspected ischemic heart disease is diagnosed as having normal SPECT, annual hardcardiac events is 0.6% / per year [22]. The annual hard event rate in asymptomatic patients with type 2 diabetes is 0.8% / year [23]. The patients with normal myocardial perfusion imaging can recommend to be managedas having a low risk of cardiac event [22-23]. Coronary intervention to the patient without ischemia further may become harmful results in terms of the prognosis. Cardiac event risk could be estimated using myocardial perfusion imaging defect score and left ventricular ejection fraction in conjunction of other clinical information [24]. Thus myocardial perfusion imaging is to help physicians in risk stratification of each patient rather than identifying a per-coronary artery lesions. And we should treat invasively the particular patient with reduced myocardial blood flow reserve [25].
4. Fusion Imaging of CT Angiography and SPECT
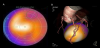
Contrast CT coronary angiography is widely used in clinical setting. A multi-slice CT with eight-detector-low had emerged in early 2000, the diagnostic sensitivity of coronary CT angiography was 75% when compared to the standard invasive coronary angiography as a reference [4]. CT coronary angiography had advanced then from 16, 32, and 64 to 320 detectors. The diagnostic performance of coronary CT angiography when compared to invasive coronary angiography has been has been proved to be eligible in many studies with a high specificity. By extracting the coronary arteries obtained from the CT coronary angiography, it is possible to create a fused image of the myocardial perfusion SPECT and CT coronary angiography even if the manufacturers of the SPECT and CT were different [8,26]. Organic narrowing lesions of a right coronary artery caused a mild ischemia in the basal inferior wall area of the left ventricle in the case of Figure 2. Culprit coronary artery lesions can be de determined to be the middle right coronary artery in a definitive diagnosis. The perfusion abnormalities in a 83-year-old male with coronary artery bypass surgery could be demonstrated to be due to high lateral branch of the left anterior descending coronary artery, by the fusion imaging (Figure 3). Thus the fusion image enabled the diagnosis of the dominant region of the blood vessel, even after bypass surgery [8].
5. The Benefits of Fusion Imaging
Fused SPECT/CT imaging provides an additional clinical value in deciding the strategy of the treatment for the patients with coronary artery disease, as well as inflammatory disease (fugure). The matched finding of ischemia and stenosis indicates a higher incidence of major adverse cardiac events (MACE) [26]. The incidence of MACE in subjects with the unmatched findings was significantly lower than that in matched subjects. Furthermore, when both perfusion and anatomical coronary arteries were normal, the MACE incidence of subjects is the lowest [27-28]. Performing a coronary intervention treatment to the stenoticvessels responsible for ischemia, which were identified by fusion imaging, has a merit of reducing the occurrence of the patient's MACE and improving the prognosis. The fusion imaging is proved to have the advantage that allows the identification of a side-branch ischemia in patients with ischemic heart disease [8,26]. However, it is important to read the fusion imaging in familiar with divergence and microcirculation disorders of the coronary arteries, as previously described [13]. The assessment that ischemia is associated with coronary stenosis by the fusion imaging matching, is extremely important in considering the coronary intervention treatment strategy (Figure 1).
6. The Coronary Artery Calcification Evaluation by SPECT / CT
Recently a hybrid SPECT / CT has been introduced and available in clinical evaluation of perfusion and coronary calcification [11,29]. The coronary calcification score can be used to estimate the total magnitude of atherosclerotic burden of the coronary arteries. A hybrid SPECT/CT system provides subclinical information of the risk of the patients. The higher the calcification score, the more possibilities of ischemia or infarction exist.
Since myocardial perfusion by SPECT can display a relative perfusion image, balanced ischemia such as multi-vessel coronary arteries may be determined to as ischemia and considered to be normal. However, coronary calcification evaluation may provide additional information. Coronary artery calcification could suggest that the inflammatory lesions had been present previously in the coronary arteries. If severe calcification were observed in patients with score more than 1000 in even normal SPECT, the patients would be considered to have the risk of coronary artery disease. Previous studies demonstrated that it would become possible to carry out improved effective screening by using a combination calcification score and myocardial perfusion SPECT [7,29]. The study showed that the subjects with higher calcium score more than 1000 had a trend toward ischemia and infarction [11]. The documentation of coronary calcification as a marker of coronary atherosclerosis can be used to manage the patients with coronary risk factors. Coronary active inflammation observed from the information of FDG-PET may indicateunstable plaque leading to plaque rapture and acute coronary syndrome.
7. Fusion Diagnosis of Functional Information and Blood Flow
The exercise or pharmacological stress induces the ischemia, resulting in transient left ventricular cavity dilatation, left ventricularsystolic or diastolic function [30]. Gated SPECT detects these functional changes of left ventricular volumes and ejection fraction. Post-stress dysfunction provides us a diagnostic clue in patients with multi-vessel disease [30-31]. Utilizing these functional information as well as myocardial perfusion, diagnosis of balanced ischemia would become possible. And the transient ischemic dilatation and post-stress dysfunction are the clinical indicators for poor prognosis of ischemic heart disease patients [30]. Multifocal collimators with dedicated reconstruction software and CT have been introduced [9]. This IQ-SPECT system with 99mTc or 201Tl shortens acquisition times and is clinically applicable in diagnosing patients with high image quality [9]. The cadmium zink-telluride (CZT) cameras provide shorter scan times and higher temporal and spatial resolution than Anger camera [32-33]. An experimental pig model reported that the quantification of absolute myocardial blood flow (MBF) measurement could become possible using 99mTc agents and 201Tl [32]. Fractional flow reserve (FFR) is a clinical indicator for the decision-making of coronary intervention. It may provide better information than angiography alone [34]. Dynamic SPECT (D-SPECT)imaging during first pass of a tracer was attained with the use of CZT camera [33]. Although PET plays a major role in precise evaluation of myocardial flow reserve using 13N-ammonia, 82Rb, 15O-water and 18f-flupiridaz [35-36], myocardial perfusion can be measured in many facilities and enhance the quantitative properties. SPECT quantification may really improve the diagnostic accuracy including the detection of balanced ischemia. The main disadvantage of SPECT in quantification may be underestimation of myocardial flow reserve when compared to that with PET. This limitation of underestimation comes from the lower extraction of 99mTc agents at high flow.
8. Conclusion
In the past few years, nuclear cardiology techniques made a great advancement, including fusion images and SPECT / CT, and have greatly changed by the appearance of a short time acquisition time. The novel hybrid system and fusion imaging to diagnose together with anatomical and functional data provides essential information in considering the therapeutic strategy of coronary intervention.
Competing Interests
The authors declare that they have no competing interests.
Author Contributions
The author substantially contributed to the literature review, drafting the manuscript and approve the final version of the manuscript.