1. Introduction
A 32 yr old patient with a past medical history positive for multiple injuries caused by a motorbike accident that happened in 1994: fracture of the femur, left kneecap, spleen; hemothorax with contusion on the left lung; spinal cord injuries (listesis, without vertebral fractures, at T11 –T12 level).
After this event he has had the following operations: femur and left kneecap osteo-sinthesis, splenectomy, left lung multiple parenchymatous resections, stabilization of the vertebral column, positioning of an endovascular prosthesis at the level of the ascending arch of the aorta. From his first day of hospitalization, he was paraplegic in intensive care unit (ICU) with an anaesthetic level lower T12 and spasticity at lower limbs. After 45 days in ICU he had been admitted in an orthopaedic ward where he stayed for two weeks and then in physiotherapy wards for several months.
Afterwards he had a bilateral operation to the Achilles tendon, braces were made for his legs and the vertebral plates removed.
For the treatment of leg spasticity he undertook, in succession, three intrathecal baclofen infusion internal pump implantations because of the periodic discharching of the pump battery (every pump had an average life of nearly five years).
At the next change, because of the constant coupling dosageeffect of Baclofen (around 150 cg/die) in the years, it was thought to lengthen the periods of pump reloading implanting a new fixed flow mechanical pump (Isomed 35 ml, vel. 0.5 ml/die) with a 15 ml higher volume than the former electronic pumps implanted. After few days it happened that the daily Baclofen dosage didn’t have the constant therapeutic effect, in terms of muscle relaxation, and it had to be adjusted continuously with multiple pump refill during the week for the achieving a higher dosage. So we witnessed a Baclofen escalation dosage up to over 1350 mcg/die [1].
2. Materials and Methods
It was controlled, with dorsal spine x-ray, without the evidence of any abnormal findings, the subarachnoid catheter connected to the pump; it resulted to have been inserted at L3-L4 level with the tip at T10 level.
In the operating room, under fluoroscopic guidance, through contrast medium injection, it has been performed a diagnostic test that has given an image suggestive of regular spreading of the contrast medium in the spinal fluid.
Thinking that it would have been easier to regulate the infusion rate of Baclofen, so changeable, with a programmable pump, the mechanical pump has been explanted and a bigger, 40 ml volume, electronic one, has been implanted.
The failure to find the proper dosage of Baclofen made it necessary to investigate, with more sophisticated imaging diagnostic tools, the spreading of the contrast medium out of the tip of the subarachnoid catheter.
At first, with the patient lying down, a mielography has been performed. It showed a suggestive distribution of contrast medium just in the rear part of the vertebral canal and it didn’t show any faded spreading in the whole section of the vertebral canal. Subsequently it was decided to visualize dorsal spine by means of CT scan during the infusion of contrast medium through the bolus port of the pump.
3. Results and Discussion
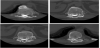
CT scan showed a posterior spreading, in the vertebral canal, of contrast medium, compatible with a diffusion in the rear subdural space. The physiopathological explanation of this event resides in the fact that the catheter hasn’t been changed, in all these years, from the first implant of the pump, and its tip, decubitating at the dura level, created a fistula into the subdural space. The contrast medium draws a distribution that goes from the catheter into the subdural space and then again into the subarachnoid space above and below the catheter tip. This determined a continuous adjustment (increment) of Baclofen dosage without having a steady therapeutic effect.
So, with the Neurosurgeon, we changed the subarachnoid catheter and implanted a new one. Eventually the therapeutic dosage of Baclofen turned back to 150 mcg/die from the first days after the catheter change and this dosage remained constant up today (already 6 months after surgery) (Figure 1).
The figure demonstrates the catheter in the subarachnoid space. In the sagittal view, the arrow identifies a well-defined fuse shaped area of contrast medium that collects in an anomalous way in the rear subdural space instead of the subarachnoid space (Figure 2 and Figure 3).
4. Conclusion
The efficacy of intrathecal baclofen has been supported by various studies [2,9-11]. The mostfrequent complications include infections, CSF leaks, and catheter malfunctions. Recently also other kind of complications, related to subarachonid infusion pump, have been reported: for istance the caudocranial fractured intrathecal catheter migration [12]. In literature there are just few descriptions of dura fistula, as possible complication from subarachnoid catheters long stay. So it is not reported the real incidence of subarachnoid catheter tip fistula in the subdural space. As soon as it becomes necessary a continuous dosage adjustment, counteracting the swinging of the therapeutic effect, of intrathecal drug, that had remained steadily efficacious for years in the past, one should suspect that a fistula between catheter tip and subdural space has been realized. It should be considering changing the subarachnoid catheter when there is a strong clinical dubt of an improper drug spreading in spinal canal confirmed by diagnostic imaging exams.
Competing Interests
The authors declare that they have no competing interests. MM belongs to the editorial board.
Author Contributions
MB: Concept and design, analysis of data.
MM Analysis of data and draft the manuscript.