1. Theoretical and Research Basis for Treatment
Substance use disorders (SUDs) are distinct conditions characterized by recurrent maladaptive use of psychoactive substances associated with significant distress. These disorders are highly common with lifetime rates of substance use or dependence estimated at over 30% for alcohol and over 10% for other substances [1,2]. Changing substance use patterns and evolving psychosocial and pharmacologic treatments modalities have necessitated the need to substantiate both the efficacy and cost effectiveness of these interventions.
Evidence for the clinical application of cognitive behavioural therapy (CBT) for substance use disorders has grown significantly [3-8]. Moreover, CBT for substance use disorders has demonstrated efficacy both as a monotherapy and as part of combination treatment [7]. CBT is a time-limited, problem-focused, intervention that seeks to reduce emotional distress through the modification of maladaptive beliefs, assumptions, attitudes, and behaviours [9]. The underlying assumption of CBT is that learning processes play an imperative function in the development and maintenance of substance misuse. These same learning processes can be used to help patients modify and reduce their drug use [3].
Drug misuse is viewed by CBT practitioners as learned behaviours acquired through experience [10]. If an individual uses alcohol or a substance to elicit (positively or negatively reinforced) desired states (e.g. euphorigenic, soothing, calming, tension reducing) on a recurrent basis, it may become the preferred way of achieving those effects, particularly in the absence of alternative ways of attaining those desired results. A primary task of treatment for problem substance users is to (1) identify the specific needs that alcohol and substances are being used to meet and (2) develop and reinforce skills that provide alternative ways of meeting those needs [10,11].
CRA is a broad-spectrum cognitive behavioural programme for treating substance use and related problems by identifying the specific needs that alcohol and or other substances are satisfying or meeting. The goal is then to develop and reinforce skills that provide alternative ways of meeting those needs. Consistent with traditional CBT, CRA through exploration, allows the patient to identify negative thoughts, behaviours and beliefs that maintain addiction. By getting the patient to identify, positive non-drug using behaviours, interests, and activities, CRA attempts to provide alternatives to drug use. As therapy progresses the objective is to prevent relapse, increase wellness, and develop skills to promote and sustain well-being. The ultimate aim of CRA, as with CBT is to assist the patient to master a specific set of skills necessary to achieve their goals. Treatment is not complete until those skills are mastered and a reasonable degree of progress has been made toward attaining identified therapy goals. CRA sessions are highly collaborative, requiring the patient to engage in ‘between session tasks’ or homework designed reinforce learning, improve coping skills and enhance self efficacy in relevant domains.
The use of the Community Reinforcement Approach is empirically supported with inpatients [12,13], outpatients [14-16] and homeless populations (Smith et al., 1998). In addition, three recent metaanalytic reviews cited CRA as one of the most cost-effective treatment programmes currently available [17,18].
A-CRA is a evidenced based behavioural intervention that is an adapted version of the adult CRA programme [19]. Garner et al [19] modified several of the CRA procedures and accompanying treatment resources to make them more developmentally appropriate for adolescents. The main distinguishing aspect of A-CRA is that it involves caregivers—namely parents or guardians who are ultimately responsible for the adolescent and with whom the adolescent is living.
A-CRA has been tested and found effective in the context of outpatient continuing care following residential treatment [20-22] and without the caregiver components as an intervention for drug using, homeless adolescents [23]. More recently, Garner et al [19] collected data from 399 adolescents who participated in one of four randomly controlled trials of the A-CRA intervention, the purpose of which was to examine the extent to which exposure to A-CRA procedures mediated the relationship between treatment retention and outcomes. The authors found adolescents who were exposed to 12 or more A-CRA procedures were significantly more likely to be in recovery at follow-up.
Combining A-CRA with relapse prevention strategies receives strong support as an evidence based, best practice model and is widely employed in addiction treatment programmes. Providing a CBT-ACRA therapeutic approach is imperative as it develops alternative ways of meeting needs and thus altering dependence.
2. Case Introduction
Alan is a 17 year-old male currently living in County Dublin. Alan presented to the agency involuntarily and as a requisite of his Juvenile Liaison Officer who was seeing him on foot of prior drugs arrest for ‘possession with intent to supply’; a more serious charge than a simple ‘drugs possession’ charge. As Alan had no previous charges he was placed on probation for one year. This was Alan’s first contact with the treatment services. A diagnostic assessment was completed upon entry to treatment and included completion of a battery of instruments comprising the Maudsley Addiction Profile (MAP), The World Health Organization Alcohol, Smoking and Substance Involvement Screening Test (ASSIST) and the Beck Youth Inventory (BYI) (see appendices for full description of outcome measures) (Table 1).
3. Diagnostic Criteria
The apparent symptoms of substance dependency were: (1) Loss of Control - Alan had made several attempts at controlling the amounts of cannabis he consumed, but those times when he was able to abstain from cannabis use were when he substituted alcohol and/or other drugs. (2) Family History of Alcohol/Drug Usage - Alan’s eldest sister who is now 23 years old is in recovery from opiate abuse. She was a chronic heroin user during her early adult years [17-21]. During this period, which corresponds to Alan’s early adolescent years [12-15] she lived in the family home (3) Changes in Tolerance - Alan began per day. At presentation he was smoking six to eight cannabis joints daily through the week, and eight to twelve joints daily on weekends.
4. Psychosocial, Medical and Family History
At time of intake Alan was living with both of his parents and a sister, two years his senior, in the family home. Alan was the youngest and the only boy in his family. He had two other older sisters, 5 and 7 years his senior. He was enrolled in his 5th year of secondary school but at the time of assessment was expelled from all classes. Alan had superior sporting abilities. He played for the junior team of a first division football team and had the prospect of a professional career in football. He reported a family history positive for substance use disorders. An older sister was in recovery for opiate dependence. Apart from his substance use Alan reported no significant psychological difficulties or medical problems. His motives for substance use were cited as boredom, curiosity, peer pressure, and pleasure seeking. His triggers for use were relationship difficulties at home, boredom and peer pressure. Pre-morbid personality traits included thrill seeking and impulsivity (Table 2).
5. Case Conceptualisation
A CBT case formulation is based on the cognitive model, which hypothesizes that "a person’s feelings and emotions are influenced by their perception of events". It is not the actual event that determines how the person feels, but rather how they construe the event (Beck, 1995 p14). Moreover, cognitive theory posits that the “child learns to construe reality through his or her early experiences with the environment, especially with significant others” and that “sometimes these early experiences lead children to accept attitudes and beliefs that will later prove maladaptive”[24]. A CBT formulation (or case conceptualisation) is one of the key underpinnings of Cognitive Behavioural Therapy (CBT). It is the ‘blueprint’ which aids the therapist to understand and explain the patient’s’ problems.
Formulation driven CBT enables the therapist to develop an individualised understanding of the patient and can help to predict the difficulties that a patient may encounter during therapy. In Alan’s case, exploring his existing negative automatic thoughts about regarding school and his academic competences highlighted the difficulties he could experience with CBT homework completion. Whilst Alan was good at between session therapy assignments, an exploration of what is meant by ‘homework’ in a CBT context was crucial.
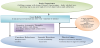
A collaborative CBT formulation was done diagrammatically together with Alan (Figure 1). This formulation aimed to describe his presenting problems and using CBT theory, to explore explanatory inferences about the initiating and maintaining factors of his drug use which could practically inform meaningful interventions.
Simmons and Griffiths et al. make the insightful observation that particular group differences need to be specifically considered and suggest that the therapist should be cognizant of the role of both society and culture when developing a formulation. They firstly suggest that the impact played by gender, sexuality and socio-cultural roles in the genesis of a psychological disorder, namely the contribution that being a member of a group may have on predisposing and precipitating factors, be carefully considered. An example they offer is the role of poverty on the development of psychological problems, such as the link evidenced between socio economic group and onset of schizophrenia. This was clearly evident in the case of Alan, who being a member of a deprived socioeconomic group, growing up and living in an area with a high level of economic deprivation, perceived that his choices for success were limited. His thinking, as an adolescent boy, was dichotomous in that he saw himself as having only two fixed and limited choices (a) being good at sport he either pursue a career as a professional sportsman or alternatively (b) he engage in crime and work his way up through the ranks as a ‘career criminal’. Simmons & Griffiths secondly suggest that being a member of a particular group can heavily influence a person’s understanding of the causality of their psychological disorder. A third consideration when developing a formulation is the degree to which being a member of a particular group may influence the acceptance or rejection of a member experiencing a psychological illness. Again this is pertinent in Alan’s case as he was part of a sub-group, a gang engaged in crime. For this cohort, crime and drug use were synonymous. Using drugs was viewed as a rite of passage for Alan.
Drug use, according to CBT models, are socially learned behaviours initiated, maintained and altered through the dynamic interaction of triggers, cues, reinforcers, cognitions and environmental factors. The application of a such a formulation, sensitive to Simmons and Griffiths (2009) aforementioned observations, proved useful in affording insights into the contextual and maintaining factors of Alan’s drug use which was heavily influenced by the availability of drugs ,his peer group (with whom he spent long periods of time) and their petty drug dealing and criminality. Similarly, engaging with his football team mates during the lead up to an important match significantly reduced his drug use and at certain times of the year even lead to abstinence. Sharing this formulation allowed him to note how his drug use patterns were driven, as per the CBT paradigm, by modifiable external, transient, and specific factors (e.g. cues, reinforcements, social networks and related expectations and social pressures).
Employing the A-CRA model allowed for this tailored fit as A-CRA specifically encourages the patient to identify their own need and desire for change. Alan identified the specific needs that were met by using substances and he developed and reinforced skills that provided him with alternative ways of meeting those needs. This model worked extremely well for Alan as he had identified and had ready access to a pro- social ‘alternative group’ or community. As he had had access to an alternative positive peer group and another activity (sport) which he was ‘really good at’, he simply needed to see the evidence of how his context could radically affect his substance use; more specifically how his beliefs, thinking and actions in certain circumstances produced very different drug use consequences and outcomes.
6. Course of Treatment and Assessment of Progress
One focus of CBT treatment is on teaching and practising specific helpful behaviours, whilst trying to limit cognitive demands on clients. Repetition is central to the learning process in order to develop proficiency and to ensure that newly acquired behaviours will be available when needed. Therefore, behavioural using rehearsal will emphasize varied, realistic case examples to enhance generalization to real life settings. During practice periods and exercises, patients are asked to identify signals that indicate high-risk situations, demonstrating their understanding of when to use newly acquired coping skills. CBT is designed to remedy possible deficits in coping skills by better managing those identified antecedents to substance use. Individuals who rely primarily on substances to cope have little choice but to resort to substance use when the need to cope arises. Understanding, anticipating and avoiding high risk drug use scenarios or the “early warning signals” of imminent drug use is a key CBT clinical activity.
A major goal of a CBT/A-CRA therapeutic approach is to provide a range of basic alternative skills to cope with situations that might otherwise lead to substance use. As ‘skill deficits’ are viewed as fundamental to the drug use trajectory or relapse process, an emphasis is placed on the development and practice of coping skills. A-CRA was manualised in 2001 as part of the Cannabis Youth Treatment Series (CYT) and was tested in that study [21] and more recently with homeless youth [23]. It was also adapted for use in a manual for Assertive Continuing Care following residential treatment [20].
There are twelve standard and three optional procedures proposed in the A-CRA model. The delivery of the intervention is flexible and based on individual adolescent needs, though the manual provides some general guidelines regarding the general order of procedures. Optional procedures are ‘Dealing with Failure to Attend’, ‘Job-Seeking Skills’, and ‘Anger Management’. Standard procedures are included in table 3 below. For a more detailed description of sessions and procedures please see appendices.
Smith and Myers describe the theoretical underpinnings of CRA as a comprehensive behavioural program for treating substance-abuse problems. It is based on the belief that environmental contingencies can play a powerful role in encouraging or discouraging drinking or drug use. Consequently, it utilizes social, recreational, familial, and vocational reinforcers to assist consumers in the recovery process. Its goal is to essentially make a sober lifestyle more rewarding than the use of substances. Interestingly the authors note: ‘Oddly enough, however, while virtually every review of alcohol and drug treatment outcome research lists CRA among approaches with the strongest scientific evidence of efficacy, very few clinicians who treat consumers with addictions are familiar with it’. ‘The overall philosophy is to promote community based rewarding of non drug-using behaviour so that the patient makes healthy lifestyle changes’ p.3[25].
A-CRA procedures use ‘operant techniques and skills training activities’ to educate patients and present alternative ways of dealing with challenges without substances. Traditionally, CRA is provided in an individual, context-specific approach that focuses on the interaction between individuals and those in their environments. A-CRA therapists teach adolescents when and where to use the techniques, given the reality of each individual’s social environment. This tailored approach is facilitated by conducting a ‘functional analysis’ of the adolescent’s behaviour at the beginning of therapy so they can better understand and interrupt the links in the behavioural chain typically leading to episodes of drug use. A-CRA therapists then teach individuals how to improve communication and other skills, build on their reinforcers for abstinence and use existing community resources that will support positive change and constructive support systems.
A-CRA emphasises lapse and relapse prevention. Relapseprevention cognitive behavioural therapy (RP-CBT) is derived from a cognitive model of drug misuse. The emphasis is on identifying and modifying irrational thoughts, managing negative mood and intervening after a lapse to prevent a full-blown relapse [26]. The emphasis is on development of skills to (a) recognize High Risk Situations (HRS) or states where clients are most vulnerable to drug use, (b) avoidance of HRS, and (C) to use a variety of cognitive and behavioural strategies to cope effectively with these situations. RPCBT differs from typical CBT in that the accent is on training people who misuse drugs to develop skills to identify and anticipate situations or states where they are most vulnerable to drug use and to use a range of cognitive and behavioural strategies to cope effectively with these situations [26].
7. Access and Barriers to Care
Alan engaged with the service for eight months. During this time he received twenty sessions, three of which were assessment focused, the remaining seventeen sessions were A-CRA focused; two of the seventeen involved his mother, the remaining fifteen were individual. As Alan was referred by the probation services, he was initially somewhat ambivalent about drug use focussed interventions. His early motivation for engagement was primarily to avoid the possibility of a custodial sentence.
8. Treatment
My sessions with Alan were guided by the principles of A-CRA [27] which focuses on coping skills training and relapse prevention approaches to the treatment of addictive disorders. Prior to engaging with Alan, I had completed the training course and commenced the A-CRA accreditation process, both under the stewardship of Dr Bob Meyers, whose training and publication offers detailed guidelines on skills training and relapse prevention with young people in a similar context [27].
During the early part of each session I focused on getting a clear understanding of Alan’s current concerns, his general level of functioning, his substance abuse and pattern of craving during the past week. His experiences with therapy homework, the primary focus being on what insight he gained by completing such exercises was also explored. I spent considerable time engaged in a detailed review of Alan’s experience with the implementation of homework tasks during which the following themes were reviewed:
-Gauging whether drug use cessation was easier or harder than he
anticipated?
-Which, if any, of the coping strategies worked best?
-Which strategies did not work as well as expected. Did he develop
any new strategies?
-Conveying the importance of skills practice, emphasising how
we both gained greater insights into how cognitions influenced his
behaviour.
After developing a clear sense of Alan’s general functioning, current
concerns and progress with homework implementation, I initiated
the session topic for that week. I linked the relevance of the session
topic to Alan’s current cannabis-related concerns and introduced the
topic by using concrete examples from Alan’s recent experience. While
reviewing the material, I repeatedly ensured that Alan understood the
topic by asking for concrete examples, while also eliciting Alan’s views
on how he might use these particular skills in the future.
Godley & Meyers [21] propose a homework exercise to accompany each session. An advantage of using these homework sheets is that they also summarise key points about each topic and therefore serve as a useful reminder to the patient of the material discussed each week. Meyers, et al. (2011) suggests that rather than being bound by the suggested exercises in the manualised approach, they may be used as a starting point for discussing the best way to implement the required skill and to develop individualised variations for new assignments [27]. The final part of each session focused on Alan’s plan for the week ahead and any anticipated high-risk situations. I endeavoured to model the idea that patients can literally ‘plan themselves out of using’ cannabis or other drugs. For each anticipated high-risk situation, we identified appropriate and viable coping skills. Better understanding, anticipating and planning for high-risk situations was difficult in the beginning of treatment as Alan was not particularly used to planning or thinking through his activities. For a patient like Alan, whose home life is often chaotic, this helped promote a growing sense of self efficacy. Similarly, as Alan had been heavily involved with drug use for a long time, he discovered through this process that he had few meaningful activities to fill his time or serve as alternatives to drug use. This provided me with an opportunity to discuss strategies to rebuild an activity schedule and a social network.
During our sessions, several skill topics were covered. I carefully selected skills to match Alan’s needs. I selected coping skills that he has used in the past and introduced one or two more that were consistent with his cognitive style. Alan’s cognitive score indicated a cognitive approach reflecting poor problem solving or planning. Sessions focused on generic skills including interpersonal skills, goal setting, coping with criticism or anger, problem solving and planning. The goal was to teach Alan how to build on his pro- social reinforcers, how to use existing community resources supportive of positive change and how to develop a positive support system.
The sequence in which these topics were presented was based on (a) patient needs and (b) clinician judgment (a full description of individual sessions may be found in appendices).
A-CRA procedures use ‘operant techniques and skills training activities’ to educate patients and present alternative ways of dealing with challenges without substances. Traditionally, CRA is provided in an individual, context-specific approach that focuses on the interaction between individuals and those in their environments. A-CRA therapists teach adolescents when and where to use the techniques, given the reality of each individual’s social environment.
9. Assessment of Treatment Outcome
A baseline diagnostic assessment of outcomes was completed upon treatment entry. This assessment consisted of a battery of psychological instruments including (see appendices for full a description of assessment measures):
-The Maudsley Addiction Profile (MAP).
-The Beck Youth Inventories.
-The World Health Organization Alcohol, Smoking and Substance
Involvement Screening Test (ASSIST).
In addition to the above, objective feedback on Alan’s clinical and drug use status through urine toxicology screens was an important part of his drug treatment. Urine specimens were collected before each session and available for the following session. The use of toxicology reports throughout treatment are considered a valuable clinical tool. This part of the session presents a good opportunity to review the results of the most recent urine toxicology screen and promote meaningful therapeutic activities in the context of the patient’s treatment goals [28].
In reporting on substance use since the last session, patients are likely to reveal a great deal about their general level of functioning and the types of issues and problems of most current concern. This allows the clinician to gauge if the patient has made progress in reducing drug use, his current level of motivation, whether there is a reasonable level of support available in efforts to remain abstinent and what is currently bothering him. Functional analyses are opportunistically used throughout treatment as needed. For example, if cannabis use occurs, patients are encouraged to analyse antecedent events so as to determine how to avoid using in similar situations in the future. The purpose is to help the patient understand the trajectory and modifiable contextual factors associated with drug use, challenge unhelpful positive drug use expectancies, identify possible skills deficiencies as well as seeking functionally equivalent non- drug using behaviours so as to reduce the probability of future drug use. The approach I used is based on the work of [28].
The Functional Analysis was used to identify a number of factors occurring within a relatively brief time frame that influenced the occurrence of problem behaviours. It was used as an initial screening tool as part of a comprehensive functional assessment or analysis of problem behaviour. The results of the functional analysis then served as a basis for conducting direct observations in a number of different contexts to attest to likely behavioural functions, clarify ambiguous functions, and identify other relevant factors that are maintaining the behaviour.
The Happiness Scale rates the adolescent’s feelings about several critical areas of life. It helps therapists and adolescents identify areas of life that adolescents feel happy about and alternatively areas in which they have problems or challenges. Most importantly it identifies potential treatment goals subjectively meaningful to the patient, facilitates positive behaviour change in a range of life domains as well as help clients track their progress during treatment.
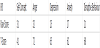
Alan’s BYI score (Table 4) indicates that at the time of assessment he was within the average scoring range on ‘self-concept’, and moderately elevated in the areas of ‘depression’, ‘anxiety’, and ‘disruptive behaviour’. His score for ‘anger’ suggested that his anger fell within the extremely elevated range. When this was discussed with Alan he agreed that this was quite accurate. Anger, and in particular controlling his anger, was subjectively identified as a treatment goal.
10. Follow-up
Given that follow-up occurred by telephone it was not feasible to administer the full battery of tests. With Alan’s treatment goals in mind it was decided to administer the MAP and ASSIST. Table 5 below illustrates Alan’s score at baseline and follow-up for the MAP and ASSIST. For summary purposes I have taken areas for concern at baseline for both instruments.
Alan’s score for cannabis was the most clinically relevant as it placed him in the 'high risk’ domain while his alcohol score indicated that he had engaged in binge drinking (6+ drinks) at T1. However, at T2 Alan’s score suggests that he had made considerable reductions in the use of both substances. Also his MAP scores for parental conflict and drug dealing suggest that he had also made major positive changes in the relevant domains of personal and social functioning as well as ceasing criminal behaviour.
At 3 months post-discharge I contacted Alan by phone. He had maintained and continued to further his progress. His drug use was at a minimal level (1 or 2 shared joints per month). He was no longer engaged in crime and his probationary period with the judicial system had passed. He had received a caution for his earlier drugs charge. At the time of follow-up he was enjoying participating in a Sports Coaching course and was excelling with his study assignments. Relationships had improved considerably with his mother and sister and he had re-engaged with a previous, positive, peer group linked to his involvement with the GAA . Overall he felt he was doing extremely well.
11. Complicating Factors with A-CRA Model
There are many challenges that may arise in the treatment of substance use disorders that can serve as barriers to successful treatment. These include acute or chronic cognitive deficits, health problems, social stressors and a lack of social resources [7]. Among individuals presenting with substance use there are often other significant life challenges including early school leaving, family conflicts, legal issues, poor or deviant social networks, etc. A particular challenge with Alan’s case was the social and environmental milieu which he shared with his drug using peers. For Alan, who initially had few skills and resources, engaging in treatment meant not only being asked to change his overall way of life but also to renounce some of those components in which he enjoyed a sense of belonging, particularly as he had invested significantly in these friendships. A sense of ‘belonging to the substance use culture’ can increase ambivalence for change [7]. Alan’s mother strongly disapproved of his drug using peer group and failed to acknowledge Alan’s perceived loss. This resulted in mother- son conflict. The use of the caregiver session allowed an exploration of perceived ‘losses’ relative to the ‘gains’ associated with Alan’s abstinence. It was moreover seen to be critical to establish alternatives for achieving a sense of belonging, including both his social connection and his social effectiveness. Alan’s sports ability allowed for this to be fostered. He is a talented sportsman which often meant his acceptance within a team or group is a given.
Despite the positive effects of A-CRA it is not without its shortcomings. The approach is at times quite American- oriented, particularly around identifying local resources and its focus on culturally specific outlets in promoting social engagement as alternatives to substance use. While this is supported in the literature, it may not necessarily be transferable to certain Irish adolescent contexts or subcultures.
12. Treatment Implications of the Case
A-CRA captures a broad range of behavioural treatments including those targeting operant learning processes, motivational barriers to improvement and other more traditional elements of cognitivebehavioural interventions. Overall, this intervention has demonstrated efficacy. Despite this heterogeneity, core elements emerge based in a conceptual model of SUDs as disorders characterized by learning processes and driven by the strongly reinforcing effects of the substances of abuse. There is rich evidence in the substance use disorders literature that improvement achieved by CBT (7) and indeed A-CRA (Godley et al. and Garner et al. [22,20]) generalizes to all areas of functioning, including social, work, family and marital adjustment domains. The present study’s finding that a reduction in substance-related symptoms was accompanied by improved levels of functioning, social adjustment and enhanced quality of life, provides further support for this point.
In conclusion, there is some preliminary evidence that A-CRA is a promising treatment in the rehabilitation of adolescent substance users in Ireland and culturally similar societies. Clearly, results from a case study have limited generalisability and there is need for larger controlled studies providing robust outcomes to confirm the efficacy of A-CRA in an Irish context. A more systematic study of this issue is in the interest of adolescent substance users and the health services providers faced with the challenge of providing affordable, evidencebased mental health and addiction care to young people.
13. Recommendations to Clinicians and Students
The ACRA model is a structured assemblage of a range of cognitive and behavioural activities (e.g. a rationale and overview of the paradigm, sobriety sampling, functional analyses, communication skills, problem solving skills, refusal skills, jobs counselling, anger management and relapse prevention) which are shared in varying degrees with other CBT approaches. The ACRA model has the advantage of established effectiveness. A foundation in empirical research together with its manual- supported approach results in it being an appropriate “off the shelf ” intervention, highly applicable to many adolescent substance misusers. Such a focussed approach also has the advantage of limiting therapist “drift”. Notwithstanding the accessible manual and other resources available on- line, clinicians and students are strongly encouraged to undergo accredited ACRA training and supervision.
Unfortunately such a structured model, despite its many advantages, does have limitations. This model may not meet the sum of all drug misusing adolescent service user treatment needs, nor is it applicable to all adolescent drug users, particularly highly chaotic individuals with high levels of co- morbidities or multi-morbidities as often found in this population [29,30]. Whilst focussing on specifically on drug use, ACRA does not directly address co-existing problem behaviours or challenges such as depression, anxiety, personality disorder, or post traumatic stress disorder (PTSD) synergistically linked to drug use. It is possible that given the high levels of dual diagnoses encountered in this population as well as the compounding effect that drug use exerts on multiple systems, clinicians and practitioners may find a strict application of the ACRA model limiting, necessitating the application of an additional range or layer of psychotherapeutic competencies? Additionally the ACRA model does not focus explicitly on other psychological activities useful in the treatment of drug misuse such as the control and management of unhelpful cognitive styles or habits; breathing or progressive relaxation skills; anger management; imagery, visualisation and mindfulness. That is, as a manual based approach comprising a number of fixed components, a major potential challenge facing clinicians and students is the tension they may experience between maintaining strict fidelity to a pure ACRA approach, versus the flexibility l approved by more formulation driven CBT approaches?
The advantages of a skilled application of a formulation driven approach which are cited and summarised in are multiple and include the collaborative nature of goal setting, the facilitation of problem prioritisation in a meaningful and useful manner; a more immediate direction and structuring of the course of treatment; the provision of a rationale for the most fitting intervention point or spotlight for the treatment; an integration of seemingly unrelated or dissimilar difficulties in a meaningful yet parsimonious fashion; an influence on the choice of procedures and “homework” exercises; theory based mechanisms to understand the dynamics of the therapeutic relationship and a sense of targeted and ‘extra-therapeutic’ issues and how they could be best explained and managed, especially in terms of precipitators or triggers, core beliefs, assumptions and automatic thoughts.
Thus given the above observations and together with the importance placed on engagement and retention, the high variability in the cognitive, emotional, social and developmental domains [4] differences in roles (e.g. teenagers who are also parents) and levels of autonomy as well as high degrees of dual diagnosis or co- morbidities found in this group [29,30] practitioners are encouraged to also develop competencies in allied psychological treatment models such as Motivational Interviewing [31]; familiarity with the core principles of CBT, disorder specific and problem-specific CBT competences, the generic and meta- competences of CBT as well as an advanced knowledge and understanding of mental health problems that will provide practitioners with the confidence and capacity to implement treatment models in a more flexible yet coherent manner,. In addition to seeking supervision and mentorship students and practitioners are directed, as a starting point, to University College London’s excellent resources outlining the competencies required to provide a more comprehensive interventions [11].
Disclosure
Both authors reported no conflict of interest in the content of this paper.
Author Contributions
Conceived and designed the experiments: JI. Recruitment & assessment and on going treatment t of patient JI. On going supervision of case KD. Contributed reagents/materials/analysis tools: JI, & KD. Wrote the paper: JI. Contributed to final draft paper KD.
Acknowledgments
We thank Adolescent Addiction Services, Health Service Executive.